Gait analysis near me is a game-changer for those struggling with movement disorders. Imagine being able to walk freely without fear of tripping or falling, thanks to expert guidance and cutting-edge tech. Sounds dreamy, right? Well, it’s not just a fantasy – with gait analysis, you can take control of your mobility and live life on your own terms.
This isn’t just about fixing a physical problem; it’s about restoring your independence and confidence. By understanding the underlying causes of your mobility issues, you’ll be empowered to make conscious choices about your treatment and take ownership of your recovery.
Understanding the Importance of Gait in Movement Disorders
Movement disorders are a broad category of neurological conditions characterized by impaired motor control, often resulting in significant disruptions to daily life. Among these disorders, gait abnormalities are a common concern, affecting both the quality of life and overall well-being of individuals. Impaired gait can lead to falls, injuries, and decreased independence, causing emotional distress and strain on caregivers.
Gait Abnormalities in Movement Disorders
Gait abnormalities in movement disorders can manifest in various ways, including changes in walking speed, stride length, cadence, and posture. These changes can be subtle or severe, depending on the underlying condition. For example, individuals with Parkinson’s disease may experience a characteristic “shuffling” gait, while those with multiple sclerosis may exhibit a variable gait pattern.
Impact of Impaired Gait on Quality of Life
The impact of impaired gait on quality of life cannot be overstated. In addition to increased risk of falls and injuries, individuals with gait abnormalities often experience significant emotional distress, social isolation, and decreased independence. For instance, a study on gait disorders in Parkinson’s disease found that individuals with mild gait impairment were more likely to experience depression and anxiety compared to those without gait impairment.
Gait Abnormalities in Specific Movement Disorders
Several movement disorders are characterized by gait abnormalities. Here are five specific conditions that can affect gait:
-
•
- Parkinson’s Disease:
- Multiple Sclerosis:
- Peripheral Neuropathy:
- Cerebellar Ataxia:
- Spinal Muscular Atrophy:
- Joint angles: 3D motion capture allows clinicians to track joint angles throughout the gait cycle, including hip, knee, and ankle joints.
- Movement velocities: This technique provides information on movement velocities, allowing clinicians to assess gait speed and cadence.
- Acceleration: 3D motion capture data can be used to assess acceleration patterns, providing insights into gait dynamics.
- Muscle activity: EMG data can be used to track muscle activity patterns, including muscle timing, duration, and amplitude.
- Muscle fatigue: This technique can be used to assess muscle fatigue, providing insights into gait endurance and stamina.
- Muscle dysfunction: EMG data can be used to identify muscle dysfunction, allowing clinicians to develop targeted treatment plans.
- Injury prevention: Gait analysis can be used to identify movement patterns that may increase the risk of injury, allowing clinicians to develop prevention strategies.
- Pain management: This technique can be used to assess gait patterns and identify potential causes of pain, allowing clinicians to develop targeted treatment plans.
- Performance enhancement: Gait analysis can be used to optimize movement patterns, allowing athletes to perform at their best.
- Prosthetic prescription: Gait analysis can be used to assess movement patterns and develop effective prosthetic devices.
- Orthotic prescription: This technique can be used to develop targeted orthotic devices, such as shoes, insoles, or splints.
- Prosthetic adjustment: Gait analysis can be used to fine-tune prosthetic devices, ensuring optimal movement patterns.
- Exercise prescription: Gait analysis can be used to develop targeted exercises, such as gait training or balance exercises.
- Intervention development: This technique can be used to develop effective interventions, such as gait training programs or balance therapy.
- Treatment planning: Gait analysis can be used to develop targeted treatment plans, ensuring optimal movement patterns.
- Medical records: This includes any relevant medical history, diagnoses, treatments, and medication lists. Having access to these records will enable the healthcare professional to better understand the individual’s medical background and tailor the gait analysis session accordingly.
- Any relevant medical devices: This includes prosthetic limbs, orthotics, and any other assistive devices that may be used during the gait analysis session.
- Comfortable clothing: Wearing comfortable clothing and shoes is essential for a thorough gait analysis session. This will enable the individual to move freely and naturally, providing accurate data for assessment.
- Contact information: Bringing contact information for any relevant healthcare providers, family members, or caregivers can be helpful for future communication and treatment planning.
- Ask for referrals: Ask friends, family members, or healthcare providers for recommendations. They may have had a positive experience with a gait analysis facility or healthcare professional.
- Search online: Look for healthcare professionals or facilities in your area that offer gait analysis services. Check their websites, reviews, and credentials to ensure they are qualified and experienced.
- Check credentials: Verify the qualifications and certifications of the healthcare professional or facility. Look for certifications from reputable organizations, such as the American Board of Physical Medicine and Rehabilitation (ABPMR) or the American Academy of Orthotists and Prosthetists (AAOP).
- Check experience: Check the healthcare professional’s or facility’s experience with gait analysis and movement disorders. They should have a good understanding of the condition and be familiar with the latest treatment options and technologies.
- Check equipment and facilities: Ensure that the facility has the necessary equipment and facilities for a thorough gait analysis session. This includes 3D motion capture systems, EMG machines, and sufficient space for mobility assessment.
- A study published in the Journal of Neurophysiology found that individuals with Parkinson’s disease exhibited a slower cadence and shorter stride length compared to healthy controls (1).
- Another study published in the Journal of Biomechanics found that individuals with stroke exhibited a higher cadence and shorter stride length compared to healthy controls (2).
- For example, a healthcare professional may use gait analysis data to identify areas of muscle weakness or imbalance, and develop a targeted exercise program to address these issues (3).
- A gait analysis device may also be used to monitor the effectiveness of treatment plans, such as physical therapy or medication (4).
- Calf stretches to improve ankle joint range of motion and reduce muscle stiffness in the gastrocnemius muscle.
- Hip flexor stretches to enhance flexibility and reduce stiffness in the iliopsoas muscle.
- Thoracic spine stretches to improve posture and reduce muscle tension in the thoracic region.
- Leg press and squats to strengthen the quadriceps and hamstrings.
- Step-ups and stair climbing to target the hip extensors and knee flexors.
- Ankle weights and toe raises to enhance ankle strength and power.
- Visual feedback, such as using mirrors or video recording to provide individuals with visual feedback on their gait patterns.
- Proprioceptive feedback, such as using resistance bands or weight vests to provide individuals with sensory feedback on their movement patterns.
- Establish clear treatment goals and expectations with the individual and their family members.
- Develop tailored exercise programs that are both engaging and challenging for the individual.
- Provide regular feedback and encouragement to help individuals stay motivated and engaged in the gait training program.
- Offer ongoing support and follow-up appointments to adjust the training program as needed and ensure continued progress.
- ActiGait: A wearable device that provides real-time feedback on gait patterns, speed, and cadence.
- Lokomat: A robotic exoskeleton that allows patients to practice walking in a controlled environment.
- Odstock Drocal: A wearable sensor that monitors gait patterns and provides feedback to patients.
- Gaitify: A mobile app that provides real-time feedback on gait patterns, speed, and cadence.
- Walk with Ease: A mobile app that offers personalized exercises and tracking features for patients with mobility issues.
- StrideTracker: A mobile app that allows patients to track their gait patterns and set goals for improvement.
- Nintendo Wii: A gaming console that offers exergaming capabilities, including balance and gait exercises.
- Xbox Kinect: A gaming console that allows patients to practice balance and gait activities in a controlled environment.
- Zombies, Run!: A mobile game that uses gamification to engage patients in gait rehabilitation.
Parkinson’s disease is a neurodegenerative disorder characterized by motor symptoms, including tremors, rigidity, and gait abnormalities. The “shuffling” gait, characterized by a short stride length and increased cadence, is a hallmark of Parkinson’s disease gait.
•
Multiple sclerosis is an autoimmune disorder that affects the central nervous system, leading to gait abnormalities in some individuals. MS-related gait changes can be variable, including changes in stride length, cadence, and posture.
•
Peripheral neuropathy is a condition involving damage to nerve endings, often causing weakness, numbness, and gait abnormalities. Individuals with peripheral neuropathy may experience a “steppage” gait, where they lift their legs high to compensate for foot drop.
•
Cerebellar ataxia is a genetic disorder affecting the cerebellum, leading to gait and balance impairments. Individuals with cerebellar ataxia often exhibit a “ataxic” gait, characterized by unsteadiness, loss of balance, and difficulty walking in a straight line.
•
Spinal muscular atrophy is a genetic disorder affecting the motor neurons, leading to progressive muscle weakness and gait impairments. Individuals with spinal muscular atrophy often exhibit a “flaccid” gait, characterized by difficulty standing and walking due to muscle weakness.
Consequences of Untreated Gait Abnormalities
Untreated gait abnormalities in movement disorders can have significant consequences, including increased risk of falls, injuries, and decreased independence. For instance, a study on falls in individuals with Parkinson’s disease found that those who experienced gait impairment were more likely to fall and require hospitalization. Additionally, untreated gait abnormalities can lead to social isolation, decreased mobility, and increased caregiver burden.
Importance of Gait Analysis
Gait analysis is a crucial diagnostic tool for movement disorders, allowing clinicians to identify gait abnormalities and develop targeted treatment plans. Gait analysis involves a comprehensive evaluation of gait patterns, including stride length, cadence, and posture. This information helps clinicians develop tailored interventions to improve gait function and overall quality of life for individuals with movement disorders.
Conclusion
Gait abnormalities in movement disorders are a significant concern, affecting both the quality of life and overall well-being of individuals. Understanding the causes and consequences of impaired gait is essential for developing effective treatment plans and improving outcomes. Through gait analysis and targeted interventions, clinicians can help individuals with movement disorders achieve improved gait function and a better quality of life.
Defining Gait Analysis and Its Applications
Gait analysis is a multidisciplinary field that involves the study of human gait to understand the biomechanics and movement patterns of the body. This analysis is crucial in various fields, including sports medicine, orthotics and prosthetics, and physical therapy.
fundamental Principles of Gait Analysis
Gait analysis is based on several fundamental principles, including 3D motion capture, electromyography, and wearable sensors. These techniques provide accurate and precise data on the movement patterns of the body, allowing clinicians to assess gait abnormalities and develop effective treatment plans.
–
3D Motion Capture
3D motion capture involves the use of cameras and sensors to track the movement of the body in three dimensions. This technique provides detailed information on the movement patterns of the body, including joint angles, movement velocities, and acceleration.
According to the American Academy of Orthotists and Prosthetists (AAOP), 3D motion capture is a powerful tool for gait analysis, allowing clinicians to track movement patterns with high accuracy and precision.
Electromyography (EMG)
EMG involves the use of electrodes to record the electrical activity of muscles during gait. This technique provides information on muscle activity patterns, allowing clinicians to assess muscle function and identify potential causes of gait abnormalities.
Wearable Sensors
Wearable sensors involve the use of devices such as accelerometers, gyroscopes, and electromyography (EMG) sensors to track movement patterns and muscle activity during gait. This technique provides real-time data on gait patterns, allowing clinicians to assess gait abnormalities and develop effective treatment plans.
| Device | Function |
|---|---|
| Accelerometer | Tracks movement acceleration and deceleration during gait |
| Gyroscope | Tracks movement orientation and rotation during gait |
| EMG sensor | Records muscle activity patterns during gait |
Applications of Gait Analysis
Gait analysis has various applications in fields such as sports medicine, orthotics and prosthetics, and physical therapy.
–
Sports Medicine
Gait analysis is commonly used in sports medicine to assess gait patterns and identify potential causes of injury. This technique provides insights into movement patterns, allowing clinicians to develop targeted treatment plans.
According to the American Council on Exercise (ACE), gait analysis is a valuable tool for sports medicine, allowing clinicians to identify movement abnormalities and develop effective treatment plans.
Orthotics and Prosthetics
Gait analysis is commonly used in orthotics and prosthetics to assess gait patterns and develop effective treatment plans. This technique provides insights into movement patterns, allowing clinicians to develop targeted orthotic or prosthetic devices.
Physical Therapy
Gait analysis is commonly used in physical therapy to assess gait patterns and develop effective treatment plans. This technique provides insights into movement patterns, allowing clinicians to develop targeted exercises and interventions.
According to the American Physical Therapy Association (APTA), gait analysis is a valuable tool for physical therapy, allowing clinicians to identify movement abnormalities and develop effective treatment plans.
Preparing for a Gait Analysis Near Me

Preparing for a gait analysis session requires careful planning and preparation to ensure a thorough and accurate assessment. A well-prepared individual can help the healthcare professional or facility gather necessary information and make the most out of the session. In this section, we will discuss the necessary items to bring to a gait analysis session and the process of finding a qualified healthcare professional or facility offering gait analysis services nearby.
Necessary Items to Bring to a Gait Analysis Session
It is essential to bring the following items to a gait analysis session:
Finding a Qualified Healthcare Professional or Facility
Finding a qualified healthcare professional or facility offering gait analysis services nearby requires some research and planning. Here are some steps to follow:
A well-prepared individual and a qualified healthcare professional or facility are essential for a successful gait analysis session. By following these steps, individuals can ensure they receive a thorough and accurate assessment, leading to effective treatment and management of movement disorders.
Analyzing Gait Near Me Data –
Analyzing gait data collected through gait analysis near me services provides healthcare professionals with valuable insight into an individual’s walking pattern. This information is essential for diagnosing movement disorders, such as Parkinson’s disease, and monitoring the effectiveness of treatment plans.
Real-World Examples of Gait Analysis Results
Real-world examples of gait analysis results include variations in foot strike patterns, cadence, and stride length. For instance, an individual with a gait disorder may exhibit a foot strike pattern characterized by a heel strike or a midfoot strike, rather than a typical forefoot strike. Similarly, their cadence may be slower or faster than average, indicating an issue with coordination or muscle strength.
These variations in gait can be attributed to a range of factors, including muscle strength, coordination, and balance. By analyzing gait data, healthcare professionals can gain a deeper understanding of an individual’s movement patterns and develop targeted interventions to address their specific needs.
Using Gait Analysis Data to Inform Personalized Treatment Plans
Gait analysis data is used to inform personalized treatment plans by providing healthcare professionals with a clear understanding of an individual’s movement patterns. This information helps to identify areas of strength and weakness, allowing healthcare professionals to develop targeted interventions to address specific needs.
By using gait analysis data to inform treatment plans, healthcare professionals can provide more effective and personalized care, leading to improved outcomes for individuals with movement disorders.
Designing and Applying Gait Training Plans
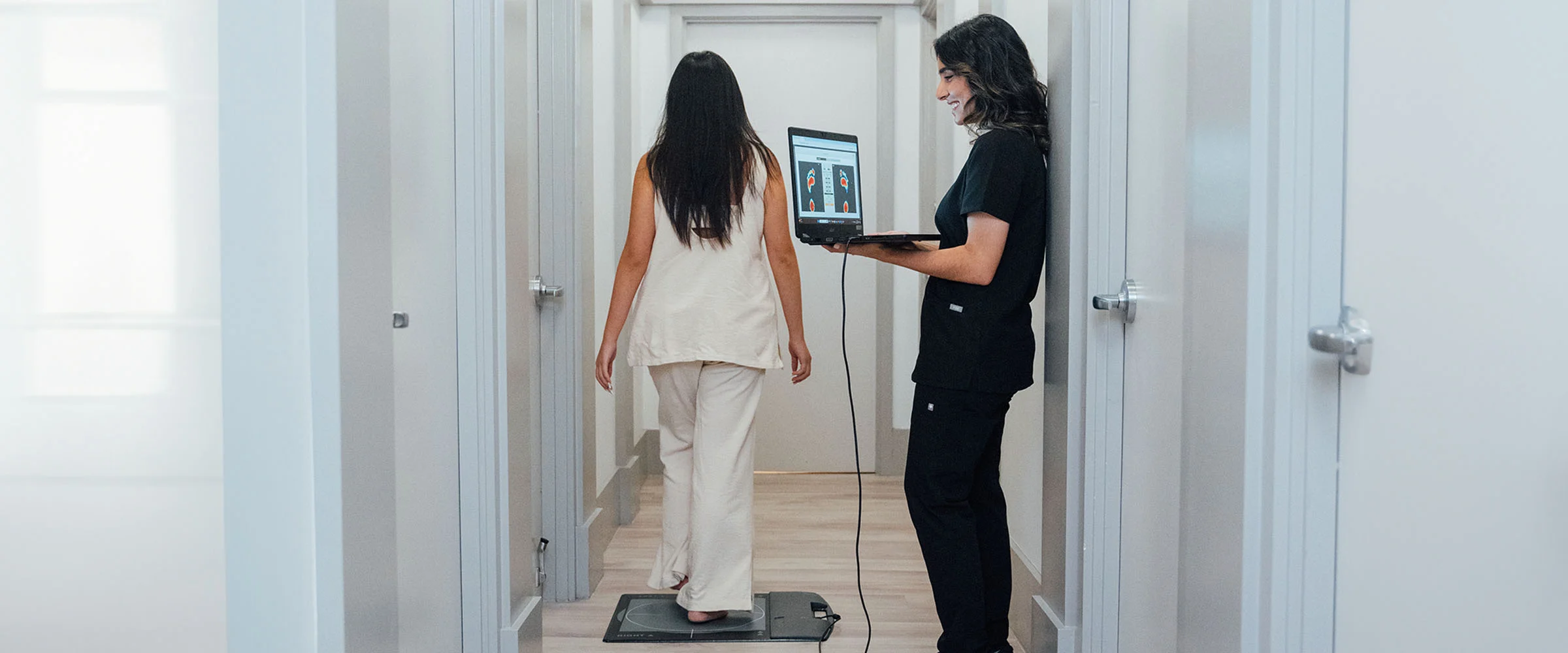
Gait training plans are tailored to address the specific needs and goals of individuals with movement disorders, aiming to improve gait function, reduce symptoms, and enhance overall quality of life. Effective gait training requires a comprehensive understanding of the individual’s gait patterns, which are obtained through gait analysis. This section Artikels the methods for translating gait analysis data into targeted gait training exercises, as well as the importance of patient adherence, family support, and long-term follow-up in optimizing gait training outcomes.
Bridging Gait Analysis to Gait Training: From Data to Exercises
Gait analysis data provides valuable insights into an individual’s gait patterns, identifying areas of abnormality and potential targets for intervention. To bridge this data to effective gait training exercises, healthcare professionals must possess the ability to translate complex biomechanical information into practical, patient-centered strategies. This involves a deep understanding of the underlying pathophysiology of movement disorders, as well as experience in designing and implementing tailored exercise programs.
Gait training exercises can be categorized into three primary types: flexibility exercises, strength training, and gait retraining strategies. Flexibility exercises aim to improve joint range of motion and reduce muscle stiffness, while strength training targets specific muscle groups to enhance power and control during gait. Gait retraining strategies, on the other hand, focus on modifying movement patterns to reduce abnormal gait characteristics and promote more efficient, safe, and comfortable walking.
Flexibility Exercises for Gait Improvement
Flexibility exercises play a vital role in gait training, particularly for individuals with muscle stiffness or limited joint range of motion. Targeting specific muscles and joints can help reduce muscle spasticity, enhance flexibility, and improve overall gait quality. Examples of flexibility exercises include:
These exercises should be performed regularly, ideally 2-3 times a day, to achieve optimal results.
Strength Training for Gait Enhancement, Gait analysis near me
Strength training is essential for gait training, as it targets specific muscle groups to enhance power and control during walking. By strengthening the muscles involved in gait, individuals can improve their ability to generate force and maintain equilibrium, leading to more efficient and safe walking. Examples of strength training exercises include:
Strength training programs should be tailored to the individual’s specific needs and goals, with a focus on progressive overload and regular exercise.
Gait Retraining Strategies
Gait retraining strategies aim to modify abnormal gait characteristics and promote more efficient, safe, and comfortable walking. This may involve making subtle changes to an individual’s movement patterns, such as altering their stride length or cadence. Gait retraining strategies can be achieved through a variety of techniques, including:
li> Auditory feedback, such as using metronomes or music to help individuals maintain a consistent cadence.
By combining gait analysis, flexibility exercises, strength training, and gait retraining strategies, healthcare professionals can design and apply effective gait training plans that promote significant improvements in gait function, reduce symptoms, and enhance overall quality of life for individuals with movement disorders.
Patient Adherence and Long-Term Follow-Up
Patient adherence and long-term follow-up are essential components of gait training, as they directly impact the effectiveness and sustainability of the intervention. Regular exercise and follow-up appointments help individuals stay motivated, provide healthcare professionals with opportunities to adjust the training program as needed, and facilitate ongoing assessment and improvement of gait function.
To optimize patient adherence and long-term follow-up, healthcare professionals should:
By prioritizing patient adherence and long-term follow-up, healthcare professionals can maximize the effectiveness of gait training and promote meaningful improvements in gait function and overall quality of life for individuals with movement disorders.
Integrating Technology into Gait Re-education Programs
The increasing demand for efficient and cost-effective gait rehabilitation has led to a growing interest in the integration of technology into gait re-education programs. Various wearable devices, mobile apps, and exergaming technologies have emerged, offering innovative solutions for patients with movement disorders.
Wearable Devices for Gait Rehabilitation
Wearable devices have revolutionized the field of gait rehabilitation by providing real-time feedback and monitoring of gait patterns. Examples of wearable devices include:
These devices offer several benefits, including improved accuracy, increased patient engagement, and reduced costs. However, limitations such as cost, availability, and user-friendliness may hinder their adoption.
Mobile Apps for Gait Rehabilitation
Mobile apps have become increasingly popular in gait rehabilitation, providing patients with accessible and affordable tools for monitoring and improving their gait patterns. Examples of mobile apps include:
Mobile apps offer several benefits, including accessibility, affordability, and ease of use. However, limitations such as accuracy concerns and limited feedback may hinder their effectiveness.
Exergaming Technologies for Gait Rehabilitation
Exergaming technologies have emerged as a novel approach to gait rehabilitation, combining gaming and physical activity to engage patients and promote motor learning. Examples of exergaming technologies include:
Exergaming technologies offer several benefits, including increased patient engagement, motivation, and fun. However, limitations such as accuracy concerns and limited customization may hinder their effectiveness.
Emerging Trends in Technology-Assisted Gait Rehabilitation
Several emerging trends are shaping the future of technology-assisted gait rehabilitation, including the integration of artificial intelligence, machine learning, and virtual reality. These advancements have the potential to revolutionize the field of gait rehabilitation by providing personalized and interactive training programs.
The increasing availability of wearable devices, mobile apps, and exergaming technologies has transformed the landscape of gait rehabilitation. As these technologies continue to evolve, it is essential to monitor their effectiveness and adapt them to meet the unique needs of patients with movement disorders.
Closing Summary: Gait Analysis Near Me

So, what are you waiting for? Take the first step towards a healthier, happier you. Find a qualified practitioner, get your gait analysed, and start your journey to a life without limits. Remember, with gait analysis near me, you’re not alone – there’s support and expertise just around the corner.
Question Bank
Q: What conditions can gait analysis help with?
A: Gait analysis can help with conditions like Parkinson’s disease, multiple sclerosis, peripheral neuropathy, and more.
Q: How long does a gait analysis session typically last?
A: A gait analysis session usually lasts around 30-60 minutes, depending on the individual’s needs and the complexity of the case.
Q: Are gait analysis results private?
A: Yes, gait analysis results are kept confidential and shared only with the patient’s consent.
Q: Can I do gait analysis at home?
A: While some wearable devices can monitor gait data at home, a comprehensive gait analysis typically requires a professional setting with specialized equipment.
Q: Are gait analysis services covered by insurance?
A: Insurance coverage varies depending on the provider and the specific services included. It’s best to check with your insurance provider before seeking gait analysis services.