As cardiovascular rehabilitation near me takes center stage, we delve into the world of comprehensive care for heart health, where expert professionals tailor treatment plans to suit each individual’s unique needs, fostering a journey of recovery, improvement, and quality of life.
In this comprehensive guide, we explore the fundamental aspects of cardiovascular rehabilitation, its importance, and the roles of healthcare professionals in developing individualized rehabilitation plans. We also discuss assessing cardiovascular risk factors, designing rehabilitation plans, implementing lifestyle modifications, monitoring progress, and the integration of advanced technologies in rehabilitation.
Understanding the Basics of Cardiovascular Rehabilitation

Cardiovascular rehabilitation is a multidisciplinary approach to treating heart and circulatory conditions, such as hypertension, heart failure, and coronary artery disease. This comprehensive program helps patients recover from interventions like coronary artery bypass grafting or heart transplantation, improving their quality of life and overall well-being.
The Importance of Cardiovascular Rehabilitation
Cardiovascular rehabilitation plays a vital role in helping patients manage their conditions and reduce the risk of complications. By incorporating exercise, education, and lifestyle modifications, patients can regain their strength, improve their cardiovascular function, and enhance their overall health.
Risks of Not Participating in Cardiovascular Rehabilitation
Not participating in cardiovascular rehabilitation can lead to a range of negative outcomes, including increased risk of:
- Cardiac complications, such as heart failure and arrhythmias
- Stroke and cerebrovascular disease
- Respiratory problems, such as chronic obstructive pulmonary disease (COPD)
- Metabolic syndrome and insulin resistance
- Poor wound healing and increased risk of infection
These complications can significantly impact a patient’s quality of life, increasing the risk of hospitalization, disability, and even death.
The Role of Healthcare Professionals in Cardiovascular Rehabilitation
A multidisciplinary team of healthcare professionals, including cardiologists, primary care physicians, physical therapists, and nurses, work together to develop and implement individualized rehabilitation plans for patients. This team approach ensures that patients receive comprehensive care, addressing their physical, emotional, and psychological needs.
Personal Stories of Recovery through Cardiovascular Rehabilitation
Real-life examples illustrate the effectiveness of cardiovascular rehabilitation in improving patients’ quality of life and overall health.
- John, a 55-year-old man, underwent coronary artery bypass grafting after experiencing a heart attack. Through cardiovascular rehabilitation, he regained his strength, improved his cardiovascular function, and returned to his job as a firefighter.
- Mary, a 62-year-old woman, was diagnosed with heart failure and underwent heart transplantation. With the help of cardiovascular rehabilitation, she improved her physical function, increased her energy levels, and resumed her hobbies, including gardening and traveling.
- David, a 40-year-old man, suffered a stroke and required physical therapy to regain his mobility. Through cardiovascular rehabilitation, he improved his balance, coordination, and strength, allowing him to return to his job as a carpenter.
These stories demonstrate the significant impact of cardiovascular rehabilitation on patients’ lives, highlighting the importance of this program in improving their quality of life and overall well-being.
Benefits of Cardiovascular Rehabilitation
The benefits of cardiovascular rehabilitation are numerous and well-documented, including:
Immediate Benefits, Cardiovascular rehabilitation near me
- Improved cardiovascular function and reduced symptoms of heart disease
- Enhanced physical strength and endurance
- Increased energy levels and improved overall health
Long-term Benefits
- Reduced risk of cardiac complications and hospitalization
- Improved mental health and reduced risk of depression and anxiety
- Increased participation in physical activity and improved overall well-being
By participating in cardiovascular rehabilitation, patients can experience these benefits and improve their quality of life.
Conclusion
Cardiovascular rehabilitation is a vital component of heart and circulatory disease management, offering numerous benefits for patients, including improved cardiovascular function, enhanced physical strength, and reduced risk of complications.
Implementing Lifestyle Modifications in Rehabilitation
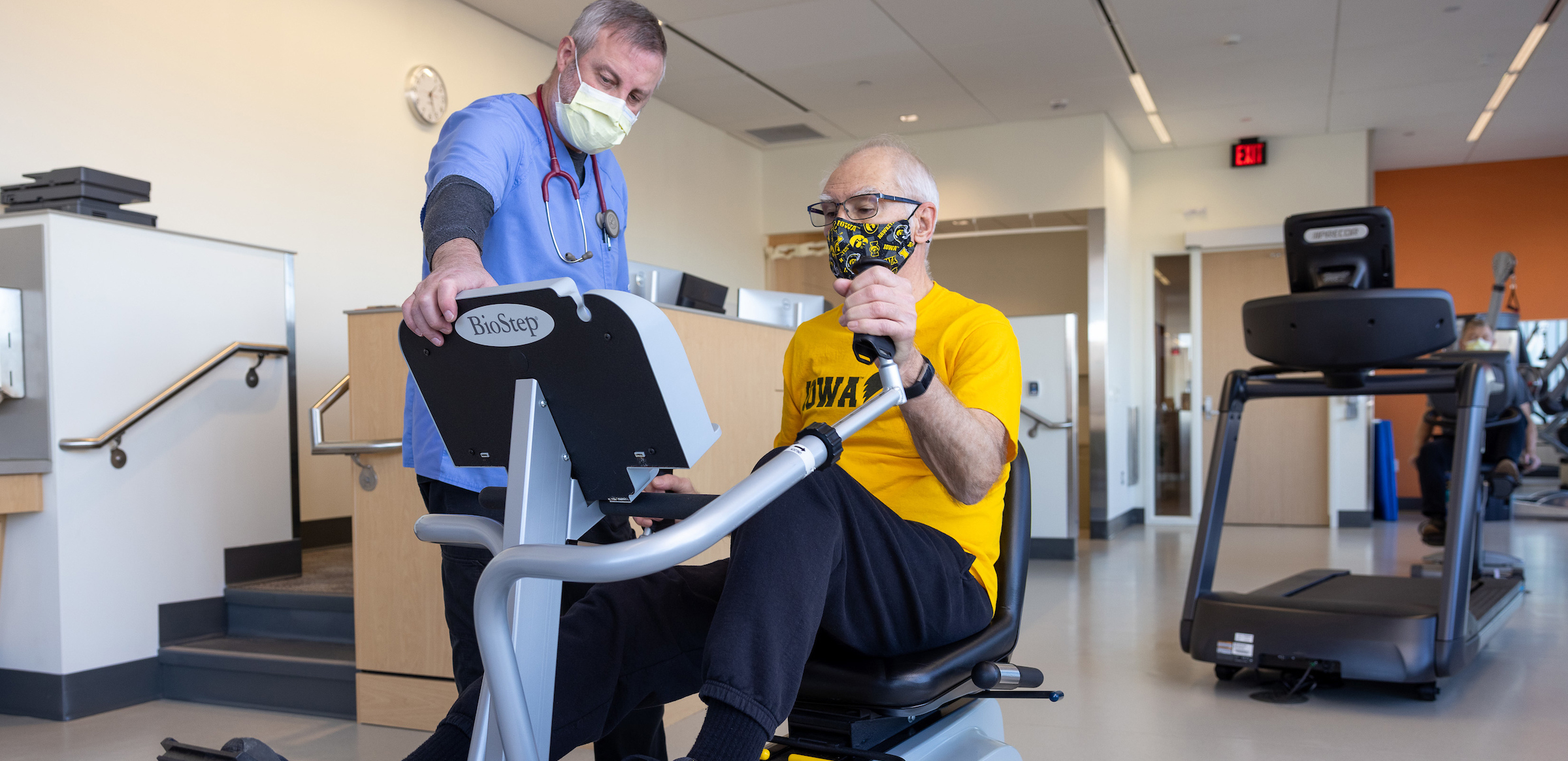
Lifestyle modifications play a crucial role in cardiovascular rehabilitation, as they can significantly improve patient outcomes and reduce the risk of chronic diseases. By adopting healthy habits, patients can regain control over their lives and improve their overall well-being.
Smoking Cessation
Smoking is a major risk factor for cardiovascular disease, as it damages the cardiovascular system and increases the risk of heart disease, stroke, and peripheral artery disease. Quitting smoking can have a profound impact on cardiovascular health, and patients should be encouraged to seek support and resources to overcome nicotine addiction. Studies have shown that quitting smoking can reduce the risk of heart disease by 50% within five years and can also reduce the risk of stroke and peripheral artery disease.
- Quitting smoking can improve cardiovascular function and reduce blood pressure.
- Smoking cessation programs and support groups can help patients overcome nicotine addiction and maintain a smoke-free lifestyle.
- Nicotine replacement therapy, such as gum or patches, can also aid in quitting smoking.
- Counseling and medication, such as bupropion or varenicline, can also be effective in helping patients quit smoking.
Stress Management
Chronic stress can have a negative impact on cardiovascular health, increasing the risk of heart disease, high blood pressure, and stroke. Stress management techniques, such as meditation, yoga, and deep breathing exercises, can help patients reduce stress and anxiety. Regular exercise and physical activity can also help reduce stress and improve overall well-being.
“Chronic stress can have a negative impact on cardiovascular health, increasing the risk of heart disease, high blood pressure, and stroke.”
Dietary Changes
A heart-healthy diet is essential for cardiovascular rehabilitation, and patients should be encouraged to adopt a Mediterranean-style diet rich in fruits, vegetables, whole grains, and lean protein sources. The Mediterranean diet has been shown to reduce the risk of heart disease, stroke, and peripheral artery disease.
| Food Group | Description |
|---|---|
| Fruits | Rich in vitamins, minerals, and antioxidants, fruits are a healthy choice for patients with cardiovascular disease. |
| Vegetables | Rich in fiber, vitamins, and minerals, vegetables are an essential part of a heart-healthy diet. |
| Whole Grains | Rich in fiber, vitamins, and minerals, whole grains are a healthy choice for patients with cardiovascular disease. |
| Lean Protein Sources | Rich in protein, low in saturated fat, lean protein sources are an ideal choice for patients with cardiovascular disease. |
Regular Exercise
Regular exercise is essential for cardiovascular rehabilitation, as it can improve cardiovascular function, reduce blood pressure, and increase overall well-being. Aerobic exercise, strength training, and flexibility exercises are all essential components of a heart-healthy exercise program.
- Aerobic exercise, such as brisk walking, swimming, or cycling, can improve cardiovascular function and reduce blood pressure.
- Strength training, such as weightlifting or resistance band exercises, can help build muscle mass and improve overall strength.
- Flexibility exercises, such as stretching or yoga, can help improve flexibility and reduce muscle tension.
- Patients should aim for at least 150 minutes of moderate-intensity aerobic exercise per week, with strength training exercises performed 2-3 times per week.
Medication Adherence and Side Effects Management
Medication adherence is critical for patients with cardiovascular disease, as it can improve treatment outcomes and reduce the risk of complications. Patients should be encouraged to take their medications as prescribed and to report any side effects to their healthcare provider.
- Adherence to medication regimens can improve treatment outcomes and reduce the risk of complications.
- Patients should discuss any side effects or concerns with their healthcare provider.
- Medication side effects should be managed with the guidance of a healthcare provider.
Monitoring Progress and Adjusting Rehabilitation Plans
Regular monitoring and feedback are essential components of cardiovascular rehabilitation. This process enables healthcare professionals to assess patient progress, identify areas for improvement, and make necessary adjustments to the rehabilitation plan. By doing so, they can ensure that patients receive the most effective and personalized care possible.
Using Clinical Metrics and Patient Self-Reporting Tools
Clinical metrics and patient self-reporting tools are widely used to assess patient progress during cardiovascular rehabilitation. Clinical metrics include parameters such as blood pressure, heart rate, and electrocardiogram (ECG) readings. These metrics provide objective measures of a patient’s physical condition and can be used to track changes over time.
On the other hand, patient self-reporting tools involve asking patients to rate their symptoms, functional status, and overall quality of life. These tools help healthcare professionals understand the patient’s subjective experience and identify areas where they may need additional support.
- Blood pressure measurements can be used to track changes in a patient’s cardiovascular health. A significant decrease in blood pressure may indicate that a patient’s rehabilitation plan is effective, whereas a plateau or increase may suggest that the plan needs to be adjusted.
- ECG readings can help identify abnormalities in a patient’s heart rhythm. Changes in ECG readings can indicate that a patient is responding to rehabilitation or that their cardiac health is deteriorating.
- Patient self-reporting tools can help clinicians identify issues that may not be apparent through clinical metrics alone. For example, a patient may report difficulty performing daily activities, despite having normal blood pressure readings.
Adjusting Rehabilitation Plans based on Patient Progress
When a patient demonstrates significant improvements in their cardiovascular health, their rehabilitation plan may need to be adjusted to accommodate their increased fitness levels. One strategy is to shift from aerobic exercise to high-intensity interval training (HIIT). HIIT involves short bursts of high-intensity exercise followed by periods of rest or low-intensity exercise.
By introducing HIIT into a patient’s rehabilitation plan, healthcare professionals can challenge patients physically and promote further improvements in cardiovascular health.
- HIIT has been shown to be effective in improving cardiovascular function and reducing symptoms in patients with heart failure and other cardiovascular conditions.
- High-intensity exercise has been associated with significant improvements in cardiovascular function, including increased cardiac output and improved vasodilatory function.
- Patient self-reporting tools can help clinicians assess a patient’s readiness for high-intensity exercise. For example, a patient may report feeling fatigued or experiencing chest pain during exercise, indicating that their rehabilitation plan may need to be adjusted.
Involving Patients in Goal Setting and Decision-Making
Involving patients in goal setting and decision-making throughout the rehabilitation process can be beneficial for several reasons. Firstly, it allows patients to take ownership of their rehabilitation plan and become more invested in their recovery.
Secondly, it can help clinicians tailor the rehabilitation plan to meet the unique needs and goals of each patient. By involving patients in goal setting and decision-making, healthcare professionals can create a personalized plan that addresses their specific challenges and promotes their overall well-being.
Involving patients in goal setting and decision-making can improve treatment adherence and outcomes.
- Studies have shown that patients who are involved in goal setting and decision-making during rehabilitation tend to have better treatment outcomes and increased satisfaction.
- Involving patients in goal setting can help clinicians identify goals that are realistic and achievable, based on the patient’s unique circumstances.
- Patient self-reporting tools can help clinicians assess a patient’s progress towards their goals and make adjustments to the rehabilitation plan as needed.
The Role of Advanced Technologies in Cardiovascular Rehabilitation: Cardiovascular Rehabilitation Near Me

The integration of cutting-edge technologies has revolutionized the field of cardiovascular rehabilitation, offering patients a more engaging, personalized, and effective approach to recovery. By leveraging advanced technologies, healthcare professionals can monitor exercise intensity, track physical activity, and guide patients towards more heart-healthy behaviors, ultimately enhancing patient engagement and informing evidence-based care decisions.
Wearable Devices in Cardiovascular Rehabilitation
Wearable devices such as smartwatches and fitness trackers are increasingly being used in cardiovascular rehabilitation to monitor exercise intensity, track physical activity, and guide patients towards more heart-healthy behaviors. These devices use advanced sensors to track heart rate, physical activity, and other vital signs, providing a comprehensive picture of a patient’s health and wellness.
For example, smartwatches can track heart rate variability (HRV) and provide real-time feedback to patients, empowering them to make informed decisions about their exercise routine. Additionally, fitness trackers can track daily physical activity, providing patients with a clear understanding of their progress and motivating them to adopt healthier habits.
- Samsung Gear: A smartwatch that tracks heart rate, physical activity, and other vital signs, providing real-time feedback to patients.
- Fitbit Charge: A fitness tracker that tracks daily physical activity, sleep quality, and other health metrics, empowering patients to make informed decisions about their lifestyle.
Electrocardiogram (ECG) Trackers and Artificial Intelligence (AI)-Powered Monitoring Systems
Electrocardiogram (ECG) trackers and artificial intelligence (AI)-powered monitoring systems are being integrated into cardiovascular rehabilitation programs to provide more accurate and personalized monitoring. These systems use AI algorithms to analyze ECG data, identifying patterns and abnormalities that may indicate cardiovascular risk.
For example, an ECG tracker can continuously monitor a patient’s heart rate and rhythm, detecting arrhythmias or other abnormalities that may indicate cardiovascular disease. AI-powered monitoring systems can analyze large datasets, identifying trends and patterns that may not be apparent to healthcare professionals.
Artificial intelligence (AI) can analyze vast amounts of data, identifying insights that may not be apparent to humans.
Benefits of Advanced Technologies in Cardiovascular Rehabilitation
The integration of advanced technologies in cardiovascular rehabilitation has numerous benefits, including:
- Improved patient engagement: Advanced technologies provide a more engaging and interactive experience for patients, empowering them to take a more active role in their recovery.
- Enhanced adherence to rehabilitation plans: By providing real-time feedback and monitoring, advanced technologies can improve adherence to rehabilitation plans, leading to better outcomes and reduced risk of complications.
- Informed evidence-based care decisions: Advanced technologies provide healthcare professionals with access to vast amounts of data, enabling them to make more informed decisions about patient care.
Last Point
Cardiovascular rehabilitation near me isn’t just a treatment; it’s a holistic approach to heart wellness. By understanding the importance of comprehensive care, adopting tailored rehabilitation plans, and embracing lifestyle modifications, individuals can recover from conditions, reduce cardiovascular risk factors, and enhance their quality of life. Join the journey towards expert care for heart wellness today.
Question & Answer Hub
What are the common cardiovascular risk factors that healthcare professionals assess and manage during the rehabilitation process?
Common cardiovascular risk factors include age, family history, smoking, high blood pressure, high cholesterol, and obesity. These factors can impact the effectiveness of rehabilitation and should be regularly assessed and managed.
How do wearable devices contribute to cardiovascular rehabilitation?
Wearable devices enable real-time monitoring of exercise intensity, tracking of physical activity, and guiding patients towards more heart-healthy behaviors. They enhance patient engagement, improve adherence to rehabilitation plans, and inform evidence-based care decisions.
What is the significance of patient education and support systems in the rehabilitation process?
Patient education and support systems play a vital role in the rehabilitation process, as they provide counseling on lifestyle changes, medication adherence, and psychological support, ultimately increasing the effectiveness of the treatment.