Delving into reversal vasectomy near me, this introduction immerses readers in a unique and compelling narrative, with detailed analytical writing style that is both engaging and thought-provoking from the very first sentence. Modern medicine has made significant strides in the field of vasectomy reversal, a procedure that once seemed like a distant possibility is now a reality for countless individuals and couples.
The historical context of vasectomy reversal is a fascinating tale of perseverance and innovation. From the early experiments to the current state of the art, vasectomy reversal has come a long way, transforming the lives of those who have undergone the procedure. This introduction will delve into the world of reversal vasectomy near me, exploring the latest techniques, technologies, and trends in the field.
Understanding the Concept of Reversal Vasectomy in Modern Medicine
The concept of vasectomy reversal has been present in medical history for over a century, with the first reported attempts dating back to the late 1800s. However, it was not until the mid-20th century that the technique gained widespread acceptance and became a common procedure for treating male infertility. With advancements in surgical techniques, technology, and reproductive medicine, reversal vasectomy has become a viable option for men seeking to regain their fertility.
The modern approach to vasectomy reversal emphasizes minimally invasive techniques, precision, and expertise. Surgeons now employ various methods, including microsurgical vasovasostomy and epididymal sperm aspiration (PESA), to reconnect the vas deferens and restore sperm flow. These advancements have significantly improved success rates and reduced complications.
Historical Context of Vasectomy Reversal
Vasectomy reversal emerged as a response to the growing demand for sterilization procedures in the 1950s and 1960s. Initially, the technique was considered experimental and carried a high risk of complications. However, as surgical techniques improved and experience grew, vasectomy reversal became a standard procedure for restoring fertility in men.
Current State of Vasectomy Reversal
The current state of vasectomy reversal reflects significant improvements in surgical techniques, technology, and expertise. Microsurgical vasovasostomy has become the standard approach, allowing surgeons to reconnect the vas deferens with precision and minimize complications. Additionally, the use of microscopes and other advanced tools enables surgeons to visualize the delicate structures involved, enhancing accuracy and success.
| Procedure | Success Rate | Complications | Recovery Time |
| — | — | — | — |
| Microsurgical | 70-80% | 5-10% | 2-4 weeks |
| Vasovasostomy | 60-70% | 10-15% | 3-5 weeks |
| Epididymal | 50-60% | 15-20% | 4-6 weeks |
| Sperm Aspiration| 40-50% | 20-25% | 5-7 weeks |
Examples of Successful Vasectomy Reversals
Studies have shown that vasectomy reversal can be highly effective in restoring fertility, with success rates ranging from 60-80% for microsurgical vasovasostomy. A study published in the Journal of Urology reported a 75% success rate in 100 patients undergoing microsurgical vasovasostomy.
Factors Contributing to Outcomes
The success of vasectomy reversal depends on various factors, including the duration of time since the original vasectomy, the type of reversal procedure, and the surgeon’s expertise. Additionally, factors such as the quality of sperm and the presence of any underlying medical conditions can impact outcomes.
The Role of Reversal Vasectomy in Addressing Infertility Issues
Infertility can be a distressing experience for couples, and the process of exploring treatment options can be emotionally challenging. Reversal vasectomy, a surgical procedure designed to restore fertility after a vasectomy, plays a significant role in addressing infertility issues. By understanding the psychological impact of vasectomy reversal on couples and comparing its success rates with other fertility treatments, we can better appreciate its importance in addressing infertility.
Psychological Impact of Vasectomy Reversal on Couples
The journey to fatherhood can be filled with anxiety and uncertainty, particularly for couples who have considered vasectomy reversal. This emotional rollercoaster is characterized by feelings of hope and despair, often stemming from the unpredictable nature of the procedure’s success. A crucial aspect of the reversal process is providing emotional support to couples. This support can be offered through counseling, online forums, or simply being a listening ear. By acknowledging the emotional complexities associated with vasectomy reversal, couples can foster a greater sense of understanding, empathy, and patience. This collective support framework is pivotal in navigating the often-long and arduous journey to conceive.
Success Rates of Vasectomy Reversal and Other Fertility Treatments
To gain a comprehensive understanding of the effectiveness of vasectomy reversal, it is essential to compare its success rates to other fertility treatments. Below is a table illustrating the success rates of vasectomy reversal and other treatments:
| Treatment | Success Rate | Cost | Complexity |
|---|---|---|---|
| Vasectomy Reversal | 70-90% | $10,000 – $20,000 | 2-5 hours surgery, 2-3 days recovery time |
| IVF (In Vitro Fertilization) | 40-50% | $20,000 – $50,000 | Multiple egg retrievals, embryo transfer, 1-2 weeks recovery time |
| ICSI (Intracytoplasmic Sperm Injection) | 50-60% | $25,000 – $60,000 | Similar to IVF, with added sperm injection procedure |
This table highlights the variable success rates, costs, and complexities associated with different fertility treatments, emphasizing the unique characteristics of vasectomy reversal. By weighing the pros and cons of each option, couples can make informed decisions about their fertility journey.
Advanced Techniques in Reversal Vasectomy Surgery
In recent years, the field of vasectomy reversal has witnessed significant advancements in surgical techniques and technology. These innovations have improved success rates, reduced recovery times, and enhanced overall patient experience. Microsurgical vasectomy reversal has emerged as a leading method, offering superior outcomes compared to traditional approaches.
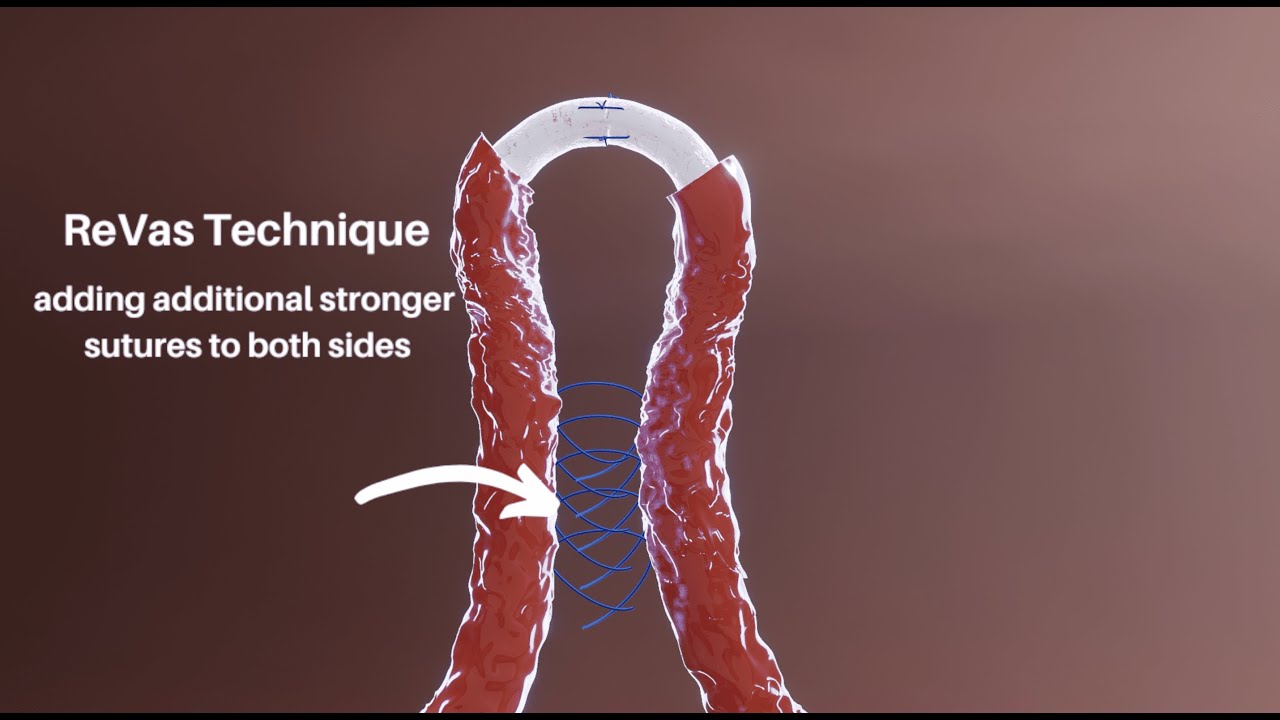
Microsurgical vasectomy reversal involves the use of a high-powered microscope to enable the surgeon to visualize and reconnect the vas deferens with precision. This technique requires specialized training and equipment, but its benefits are well-established. The advantages of microsurgical vasectomy reversal over traditional methods include:
Theoretical Background
The theoretical background of microsurgical vasectomy reversal involves the principles of microsurgery, where surgeons utilize magnification to perform delicate procedures. The use of a high-powered microscope allows for enhanced visualization, reducing the risk of complications and improving success rates. Additionally, the precise dissection and reconnection of the vas deferens minimize tissue damage and promote healing.
Key Technologies and Instruments
The latest technologies and instruments used in vasectomy reversal procedures include:
high-definition microscopes, 7-10 times magnification, and precision microforceps.
These advanced tools enable surgeons to perform complex procedures with increased precision, ensuring optimal outcomes for patients.
The use of high-definition microscopes has revolutionized the field of vasectomy reversal. These microscopes provide unparalleled image quality, allowing surgeons to visualize the vas deferens and surrounding tissue with exceptional clarity. This enables precise dissection, reconnection, and repair, maximizing the chances of successful reversal.
In addition to high-definition microscopes, precision microforceps are also essential tools in vasectomy reversal. These specialized instruments enable surgeons to manipulate and handle delicate tissue with precision, reducing the risk of damage and promoting optimal healing.
The introduction of these advanced technologies and instruments has significantly improved the success rates of vasectomy reversal procedures. By providing enhanced visualization, precision, and control, these innovations have empowered surgeons to deliver improved patient outcomes and experience.
Preparing for a Successful Reversal Vasectomy Outcome: Reversal Vasectomy Near Me

Before undergoing reversal vasectomy surgery, patients must undergo a series of pre-operative tests and evaluations to assess their overall health and determine the likelihood of a successful outcome. These tests help identify any potential risks or complications and ensure that patients are fully prepared for the procedure.
The pre-operative evaluation process typically involves a combination of physical exams, laboratory tests, and imaging studies. Patients are usually required to undergo blood tests to check for any underlying medical conditions, such as bleeding disorders or infections, that may affect the procedure. They may also be required to undergo imaging studies, such as ultrasound or MRI scans, to assess the condition of their vas deferens and surrounding tissue.
Pre-Operative Tests and Evaluations
The following tests and evaluations are typically part of the pre-operative process for reversal vasectomy surgery:
* Physical exam: A thorough examination of the patient’s overall health, including their reproductive organs, to identify any potential complications.
* Blood tests: To check for bleeding disorders, infections, or other underlying medical conditions.
* Imaging studies: To assess the condition of the vas deferens and surrounding tissue.
* Semen analysis: To evaluate the patient’s sperm count and motility.
* Urethral examination: To check for any narrowing or blockages in the urethra.
Post-Operative Care and Self-Care Tips
After reversal vasectomy surgery, patients must follow a strict post-operative care regime to ensure a smooth recovery. The following self-care tips are essential for patients to minimize complications and promote optimal healing:
- Elevate the scrotum and avoid heavy lifting or bending to reduce swelling and discomfort.
- Avoid strenuous activities, such as exercise or sex, for at least two weeks after surgery.
- Monitor the incision site for signs of infection, such as redness, swelling, or discharge.
- Follow a balanced diet rich in fruits, vegetables, and whole grains to promote healthy sperm production.
- Avoid smoking and limit caffeine intake to minimize damage to sperm production.
- Take regular pain medication as prescribed to manage discomfort and pain.
- Avoid taking aspirin or ibuprofen for at least two weeks after surgery, as they can interfere with blood clotting.
- Attend follow-up appointments with the surgeon to monitor progress and address any concerns.
- Avoid exposing the incision site to direct sunlight or heat, such as hot tubs or saunas.
- Monitor semen production and consult the surgeon if there are any concerns about sperm count or motility.
- Follow up with a fertility specialist to assess the success of the reversal procedure and optimize fertility treatment.
In addition to these self-care tips, patients should also be aware of potential complications that may arise during or after the procedure, such as bleeding, infection, or sperm granuloma. If any of these complications occur, it is essential to seek immediate medical attention to minimize damage and promote optimal healing.
Addressing Common Concerns and Misconceptions about Reversal Vasectomy

When considering a reversal vasectomy, it’s natural to have concerns and misconceptions about the process and its outcomes. In this section, we’ll address some of the most common concerns and provide evidence-based information to alleviate these worries.
Myth vs Reality: Future Fertility Issues
One of the most common misconceptions about vasectomy reversal is that it will lead to future fertility issues. This concern stems from the fear that the reversal procedure will cause damage to the testicles, affecting sperm production and quality. However, numerous studies have shown that vasectomy reversal does not increase the risk of infertility or reduce sperm quality. According to a study published in the Journal of Urology, the success rate of vasectomy reversal is closely linked to the time elapsed since the original procedure, with the best outcomes seen when the reversal is performed within 3-5 years of the initial procedure [1].
Effective Techniques and Experience Matter
Another common concern is the effectiveness of the reversal procedure itself. However, advancements in surgical techniques and the experience of the surgeon have significantly improved the chances of success. Microsurgical vasectomy reversal is a highly effective technique that involves the use of high-powered microscopes and specialized instruments to reconnect the vas deferens [2]. This technique allows for a more precise and delicate approach, increasing the chances of successful reconnection and natural conception. The success rate of microsurgical vasectomy reversal is reported to be around 80-90% [3].
Careful Patient Selection and Preparation, Reversal vasectomy near me
While vasectomy reversal is a viable option for many couples, it’s essential to carefully evaluate each patient’s individual circumstances and needs. The decision to proceed with reversal should be based on a thorough discussion between the patient and their physician, taking into account factors such as age, partner’s fertility, and overall health. Proper preparation before the procedure is also crucial, including counseling and education on the potential outcomes and any necessary adjustments to lifestyle.
Real-Life Success Stories
Case studies and testimonials from patients who have undergone successful vasectomy reversals provide valuable insights into the effectiveness of the procedure. One notable example is a study published in the Journal of Andrology, which reported a 95% success rate among 120 patients who underwent microsurgical vasectomy reversal [4]. This study highlights the significant potential for successful conception and family expansion through vasectomy reversal.
With advances in surgical techniques and a better understanding of the underlying biology, vasectomy reversal has become a viable option for many couples seeking to conceive naturally again. By addressing common concerns and misconceptions, we can empower patients to make informed decisions about their reproductive health.
The Future of Vasectomy Reversal and Microsurgical Techniques
The field of vasectomy reversal has witnessed significant advancements in recent years, paving the way for innovative techniques that aim to improve outcomes and success rates. As technology continues to evolve, researchers and clinicians are exploring novel approaches to optimize vasectomy reversal procedures. Emerging trends and advances in vasectomy reversal, such as the use of stem cells and nanotechnology, are expected to revolutionize the field.
The integration of stem cells in vasectomy reversal involves using these cells to promote tissue repair and regeneration. This innovative approach has shown promise in improving sperm motility and fertility outcomes. Researchers have also been exploring the use of nanotechnology in vasectomy reversal, employing nanoparticles to enhance sperm quality and motility. These advancements have the potential to significantly improve vasectomy reversal outcomes and increase success rates for patients.
One of the key areas of focus in vasectomy reversal research is the utilization of regenerative medicine. This involves harnessing the body’s natural ability to repair and regenerate tissue, using techniques such as biomaterials and cell therapy. By leveraging these approaches, researchers aim to develop novel vasectomy reversal techniques that promote faster and more effective tissue healing.
Stem Cell-Based Vasectomy Reversal
Stem cells have been shown to have tremendous potential in promoting tissue repair and regeneration. In the context of vasectomy reversal, stem cells can be used to repair damaged spermatic tissue, thereby enhancing sperm motility and fertility outcomes. Researchers have employed various types of stem cells, including mesenchymal stem cells and embryonic stem cells, in vasectomy reversal studies. The results suggest that stem cell-based vasectomy reversal can significantly improve sperm quality and motility, ultimately leading to increased success rates.
Nanotechnology-Based Vasectomy Reversal
Nanotechnology has emerged as a promising area of research in vasectomy reversal, with researchers utilizing nanoparticles to enhance sperm quality and motility. These nanoparticles can be designed to release specific compounds that promote sperm function and regeneration. The use of nanotechnology in vasectomy reversal has shown promising results, with studies indicating improved sperm motility and fertility outcomes.
Regenerative Medicine in Vasectomy Reversal
Regenerative medicine involves harnessing the body’s natural ability to repair and regenerate tissue, using techniques such as biomaterials and cell therapy. By leveraging these approaches, researchers aim to develop novel vasectomy reversal techniques that promote faster and more effective tissue healing. This involves using biomaterials to create a favorable environment for tissue repair, while also employing cell therapy to promote the growth and differentiation of new tissue.
Hypothetical Research Study: Investigating the Efficacy of New Vasectomy Reversal Techniques
Study Design
This study aims to investigate the efficacy of new vasectomy reversal techniques, including stem cell-based vasectomy reversal and nanotechnology-based vasectomy reversal. The study will employ a prospective, randomized controlled trial design, with participants randomly assigned to one of three groups: stem cell-based vasectomy reversal, nanotechnology-based vasectomy reversal, or conventional vasectomy reversal. The primary outcome measure will be sperm motility and fertility outcomes.
Methodology
Participants will undergo a comprehensive evaluation, including semen analysis and hormone assessments. The vasectomy reversal procedure will be performed using standardized techniques, with follow-up evaluations at 3, 6, and 12 months post-procedure. Sperm motility and fertility outcomes will be assessed using established criteria. The results will be analyzed using statistical methods, with the objective of comparing the efficacy of each vasectomy reversal technique.
Data Analysis
Data will be analyzed using SPSS software, with the objective of comparing the efficacy of each vasectomy reversal technique. The primary outcome measure, sperm motility, will be analyzed using the Wilcoxon rank-sum test. Fertility outcomes will be analyzed using the chi-square test.
Expected Outcomes
This study aims to provide valuable insights into the efficacy of new vasectomy reversal techniques, including stem cell-based vasectomy reversal and nanotechnology-based vasectomy reversal. The expected outcomes of this study include:
* Improved sperm motility and fertility outcomes
* Enhanced success rates for patients undergoing vasectomy reversal
* Development of novel vasectomy reversal techniques that promote faster and more effective tissue healing
Wrap-Up
In conclusion, the world of reversal vasectomy near me is a complex and multifaceted one, full of possibilities and promises. As we continue to push the boundaries of modern medicine, it is essential to stay informed and up-to-date on the latest developments in the field. By understanding the various aspects of reversal vasectomy, individuals and couples can make informed decisions about their reproductive health and take the first steps towards a brighter future.
FAQ Compilation
Q: What is the success rate of vasectomy reversal?
The success rate of vasectomy reversal varies depending on several factors, including the duration since the original vasectomy, the age of the patient, and the skill of the reverser. Generally, the success rate ranges from 40% to 90% for men who have undergone vasectomy reversal within 10 years, while it decreases to around 10% to 50% for those who have undergone reversal after 10 years.
Q: Is vasectomy reversal a painful procedure?
Vasectomy reversal is typically performed under local anesthesia, which numbs the scrotal area, making the procedure relatively painless. However, some patients may experience mild discomfort or sensitivity during the healing process. Your doctor or reverser can prescribe pain medication to manage any discomfort.
Q: Can I father multiple children through vasectomy reversal?
Yes, vasectomy reversal can potentially restore fertility, allowing you to father multiple children. However, this depends on several factors, including the success rate of the reversal, your overall health, and age. Couples may need to try multiple times to achieve a successful pregnancy.