Hospice nurse jobs near me –
With hospice nurse jobs near me at the forefront, this topic delves into the compassionate world of healthcare professionals dedicated to alleviating terminal illness patients’ pain and suffering. As we navigate the intricacies of hospice nursing, we’ll explore the role its nurses play in providing palliative care, the educational paths required to become a hospice nurse, and the essential skills necessary to excel in this field.
A hospice nurse’s job involves addressing the physical, emotional, and spiritual needs of patients with life-limiting illnesses, offering care in the comfort of their own homes or in a hospice facility. Key aspects of palliative care focus on symptom management, pain relief, and improving quality of life. To become a hospice nurse, one typically requires an associate’s or bachelor’s degree in nursing, training in a hospice care program, and certification as a hospice and palliative care nurse.
Understanding the Role of Hospice Nurses in Providing Palliative Care to Terminally Ill Patients Nearby

Hospice nursing plays a vital role in providing palliative care to terminally ill patients and their families. Palliative care focuses on alleviating the symptoms, pain, and stress of a serious illness, rather than curing it. Hospice nurses work closely with patients, their families, and other healthcare professionals to ensure that patients receive comprehensive care and support throughout their journey.
Pain and Symptom Management
Hospice nurses are expertly trained to manage complex pain and symptoms, often using a combination of medication, physical therapy, and other interventions. They work with patients to identify the root causes of their pain and develop personalized care plans to address it. For instance, hospice nurses may use pain medication to control pain, or employ alternative therapies like massage or acupuncture to reduce discomfort. In some cases, they may also work with patients to develop relaxation techniques, such as deep breathing or meditation, to help manage stress and anxiety.
Emotional and Spiritual Support
Beyond physical care, hospice nurses offer emotional and spiritual support to patients and their loved ones. They listen to patients’ concerns, validate their feelings, and help them express their wishes. This support can be especially crucial during the final stages of life, when patients may feel anxious, fearful, or uncertain about their future. To address these emotional needs, hospice nurses may provide counseling, offer spiritual guidance, or simply be present with patients during difficult moments.
Family and Caregiver Support
Hospice nurses also play a vital role in supporting patients’ families and caregivers. They offer guidance on how to provide hands-on care, manage medications, and navigate the healthcare system. In some cases, they may also connect patients and their families with community resources, such as respite care or support groups. By empowering families and caregivers, hospice nurses can help them feel more confident and prepared to care for their loved ones.
Palliative Care Goals and Objectives
Key aspects of palliative care that hospice nurses focus on in their daily work include:
- Improving patients’ quality of life by alleviating symptoms and managing pain
- Enhancing patients’ emotional and spiritual well-being through support and counseling
- Empowering patients and their families to make informed decisions about their care
- Coordinating care among patients, families, and healthcare professionals to ensure comprehensive support
- Addressing the complex needs of patients with multiple medical conditions or advanced illnesses
Palliative Care for Specific Needs
Hospice nurses work with patients who have a range of medical conditions, including cancer, heart failure, lung disease, and neurological disorders. They tailor their care to meet each patient’s unique needs, using evidence-based practices and a person-centered approach. To illustrate this, consider a patient with advanced cancer who requires ongoing pain management. Hospice nurses would work closely with the patient to develop a care plan that incorporates medication, therapy, and other interventions to alleviate pain and discomfort.
Essential Skills and Qualities of a Hospice Nurse
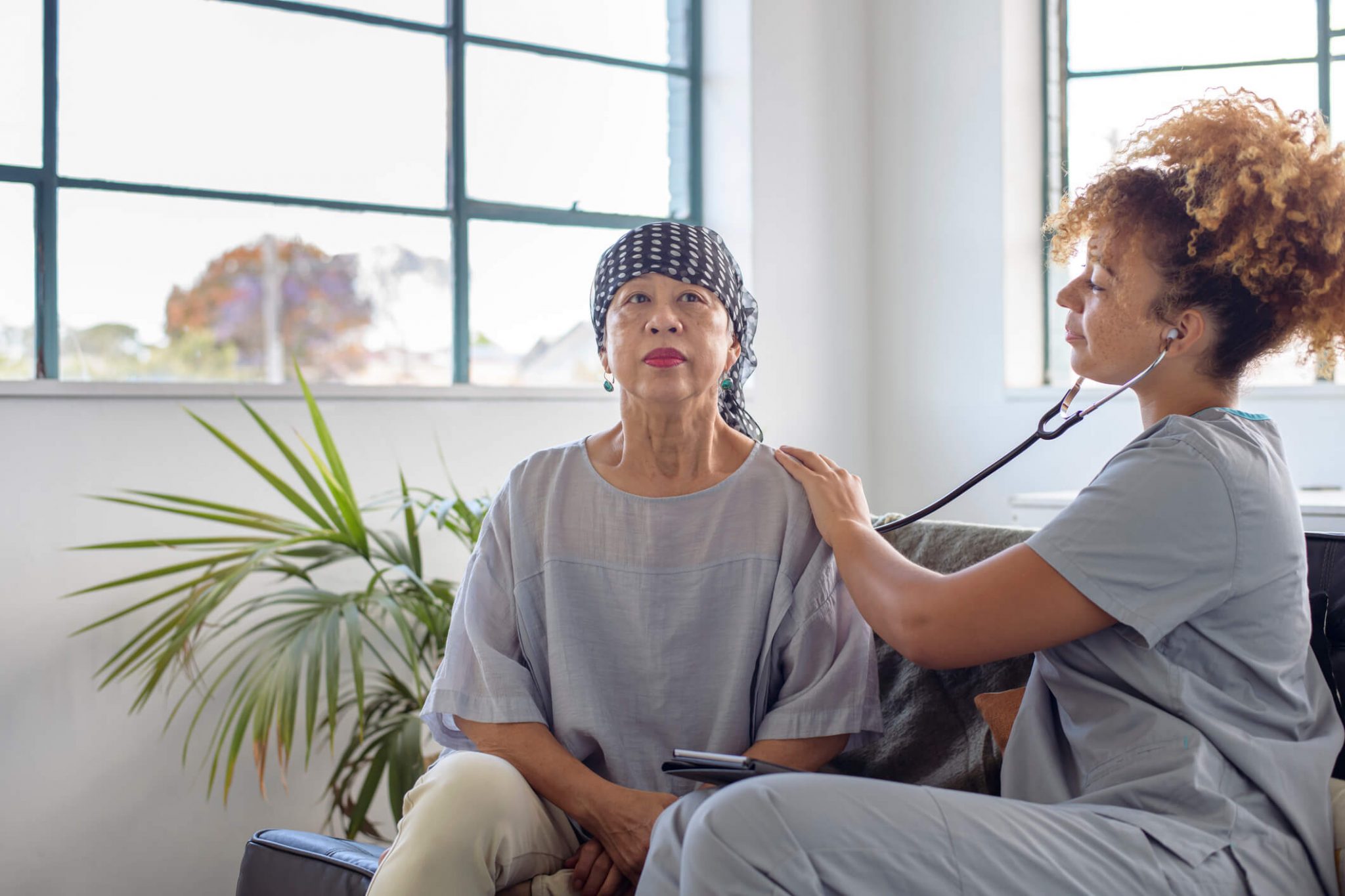
Hospice nurses play a crucial role in providing end-of-life care to terminally ill patients and their families. To fulfill this responsibility, they must possess a unique set of skills and qualities that enable them to navigate complex emotional situations with empathy, compassion, and emotional stability. Effective communication skills, emotional stability, and empathy are essential for building trust with patients and their families, and for supporting them through the final stages of their life.
Effective Coping Mechanisms for Emotionally Challenging Situations
In the field of hospice care, nurses often encounter emotionally charged situations that can be emotionally taxing. To cope with these challenges, hospice nurses can employ various strategies. For instance, mindfulness meditation can help them stay present and focused on the needs of the patient and their family. Mindfulness practices, such as deep breathing exercises and body scan meditation, can also reduce stress and anxiety. Additionally, maintaining a professional boundary can prevent burnout and emotional exhaustion. This involves setting realistic goals, prioritizing tasks, and seeking support from colleagues.
- Prioritize self-care: Engage in activities that promote relaxation and rejuvenation, such as yoga, reading, or spending time with loved ones.
- Seek support: Leverage the support of colleagues, mentors, or peers who understand the emotional demands of hospice care.
- Set realistic expectations: Establish achievable goals and prioritize tasks to prevent feelings of overwhelm and burnout.
The Importance of Emotional Stability
Maintaining emotional stability is essential for hospice nurses to provide high-quality care to terminally ill patients and their families. When hospice nurses are emotionally stable, they can remain calm and composed in challenging situations, which enables them to respond more effectively to the needs of patients and their families. Emotional stability also enables hospice nurses to empathize with patients and their families, which fosters trust and builds stronger relationships.
“The art of nursing is compassion in action.”
Empathetic Communication Skills
Empathetic communication skills are essential for hospice nurses to build trust with patients and their families. When hospice nurses employ empathetic communication skills, such as active listening and open-ended questioning, they can better understand the needs and concerns of patients and their families. This understanding enables hospice nurses to provide more effective care and support, which improves the overall quality of life for terminally ill patients and their families.
- Practice active listening: Pay close attention to patients’ and families’ concerns, and respond with empathy and compassion.
- Use open-ended questions: Encourage patients and families to share their thoughts and feelings about their care and experiences.
- Show empathy: Acknowledge patients’ and families’ emotions and show understanding through verbal and nonverbal cues.
The Value of Trust-Building
Building trust with patients and their families is critical for hospice nurses to provide effective care and support. When patients and families trust their hospice nurse, they are more likely to disclose their needs and concerns, which enables the nurse to tailor their care and support to meet these needs. Trust also fosters a sense of security and stability, which can improve patients’ and families’ quality of life.
Professional Support and Resources for Hospice Nurses Working in the Field
As hospice nurses navigate the challenges of caring for terminally ill patients and supporting families through the grieving process, it’s essential they receive professional support and resources to maintain their mental and emotional well-being. Unfortunately, this often overlooked aspect of hospice care can lead to burnout, compassion fatigue, and decreased job satisfaction.
Hospice nurses require a support system that understands the unique demands and emotional toll of their work. One valuable resource is peer support groups, where nurses can share their experiences, receive guidance, and connect with colleagues who face similar challenges. Mentorship programs also play a crucial role in helping new hospice nurses navigate the complexities of the field while providing seasoned nurses with opportunities to share their expertise.
Peer Support Groups
Peer support groups offer a safe environment for hospice nurses to discuss their feelings, share best practices, and receive support from colleagues who understand the demands of their work. These groups can be a valuable resource for:
- Nurturing emotional resilience: By sharing their experiences and connecting with colleagues, hospice nurses can build their emotional resilience and develop healthier coping mechanisms.
- Developing support networks: Peer support groups provide a platform for nurses to form meaningful connections, reducing feelings of isolation and increasing morale.
- Enhancing job satisfaction: By feeling supported and understood, hospice nurses are more likely to report higher job satisfaction and a sense of fulfillment in their work.
These benefits can have a direct impact on patient care, as nurses who feel supported and fulfilled are more likely to provide high-quality, compassionate care.
Mentorship Programs
Mentorship programs match experienced hospice nurses with newer colleagues, providing guidance, and support throughout their transition into the field. Mentorship can benefit both the mentor and mentee:
- Knowledge sharing: Seasoned nurses can share their expertise and best practices with newer colleagues, improving the overall quality of care.
- Professional growth: Newer nurses can benefit from the guidance and support of experienced mentors, accelerating their professional growth and development.
- Better patient outcomes: By sharing knowledge and expertise, mentorship programs can lead to improved patient care and outcomes.
Mentorship programs can also help to retain experienced nurses, reducing turnover rates and maintaining a stable, skilled workforce.
Local Hospice Care Organizations and Ongoing Education
Local hospice care organizations often provide ongoing education and training opportunities for their staff, ensuring they stay up-to-date on best practices, new policies, and advances in the field. These resources can benefit hospice nurses in various ways:
- Staying current: Ongoing education helps nurses stay informed about changes in the field, enabling them to provide the best possible care for patients.
- Improving skills: Training programs can enhance nurses’ clinical skills, enabling them to provide more effective care and improve patient outcomes.
- Enhancing job satisfaction: Ongoing education and training can increase job satisfaction, as nurses feel supported and empowered to provide high-quality care.
These benefits can have a positive impact on patient care, as nurses who feel supported and empowered are more likely to provide compassionate, effective care.
Managing Stress and Maintaining Mental Health, Hospice nurse jobs near me
Hospice nurses often face high levels of stress and emotional demands, making it essential they have access to resources to manage their mental health and well-being. Available resources and hotlines can provide critical support:
- National Hospice and Palliative Care Organization (NHPCO) Helpline: This hotline offers 24/7 support, connecting hospice nurses with resources and guidance from experienced professionals.
- Crisis Text Line: This free, 24/7 text line connects individuals in crisis with trained crisis counselors who can provide support and guidance.
- Employee Assistance Programs (EAPs): Many organizations offer EAPs, providing confidential support and resources for employees managing stress and emotional demands.
By acknowledging the importance of mental health and providing accessible resources, hospice care organizations can support the well-being of their nurses, ultimately improving patient care and outcomes.
The Impact of Location on Hospice Nurse Job Availability and Requirements

The profession of hospice nursing is not immune to the challenges and opportunities presented by geographical location. The availability of hospice nurse jobs, the specific requirements for these roles, and the unique challenges or opportunities that arise when working with patients from diverse cultural and socioeconomic backgrounds are all heavily influenced by location.
Urban vs. Rural Hospice Nursing Opportunities
Urban areas tend to have a higher demand for hospice nurses, with more patients and a greater number of healthcare facilities in need of qualified staff. In contrast, rural areas often face a shortage of hospice nurses, as well as other healthcare professionals, due to lower population densities and limited job opportunities. This can make it more challenging for rural hospice nurses to access professional support and resources, such as continuing education and mentorship.
Rural hospice nurses often have to navigate isolated working conditions, lacking access to colleagues and support networks
Challenges of Cross-Cultural and Socioeconomic Diversity
Hospice nurses working in areas with high levels of cultural and socioeconomic diversity may encounter unique challenges, such as language barriers, differing cultural attitudes towards death and dying, and varying levels of access to healthcare resources. For example, patients from lower socioeconomic backgrounds may face barriers to accessing hospice care due to lack of health insurance or transportation.
- Language barriers: Hospice nurses working with patients who speak little or no English may need to rely on interpreters or translation services to communicate effectively
- Cultural differences: Nurses should be aware of and respect cultural norms and values related to death and dying, such as the importance of family gatherings during the final stages of life
- Economic disparities: Nurses may need to advocate for patients who face financial barriers to accessing necessary end-of-life care, such as pain management or home care
Impact of Local Healthcare Policies and Regulations
Local healthcare policies and regulations can shape the role of hospice nurses in providing end-of-life care, dictating the types of services that can be provided, the qualifications and training required for hospice nurses, and the reimbursement rates for hospice care.
- State and local laws governing end-of-life care: Nurses should be aware of laws regulating assisted dying, advance care planning, and palliative care
- Healthcare policy and reimbursement: Nurses may need to navigate complex reimbursement systems and policy changes affecting hospice care, such as Medicare Advantage plans
- Certification and licensure: Nurses may need to meet specific certification and licensure requirements to practice hospice nursing in a particular state or region
Staying Current with the Latest Developments in Palliative Care: Hospice Nurse Jobs Near Me
As a hospice nurse, providing the best possible care for terminally ill patients is a top priority. To remain effective in this role, hospice nurses must stay current with the latest developments in palliative care. This requires ongoing education and commitment to ongoing professional development. In this section, we will explore the importance of ongoing education in the field of hospice and palliative care, the process of obtaining and maintaining certification as a hospice nurse, and the value of attending conferences and workshops for staying current on the latest trends and research in the field.
Importance of Ongoing Education in Hospice and Palliative Care
Ongoing education is essential for hospice nurses to stay current with the latest research, guidelines, and best practices in palliative care. This can include attending conferences, workshops, and seminars, as well as participating in online courses and webinars. By staying current, hospice nurses can provide the most effective and compassionate care for their patients, which can improve patient outcomes and enhance the overall quality of care. According to a study by the American Academy of Hospice and Palliative Medicine, hospice nurses who engaged in ongoing education reported improved patient outcomes and increased job satisfaction.
- New research and guidelines on pain management, symptom control, and end-of-life care
- Advancements in medical technologies and therapies, such as palliative sedation and comfort care
- Best practices for providing emotional and spiritual support to patients and families
- Current trends and innovations in hospice and palliative care, such as the use of music therapy and pet-assisted therapy
Obtaining and Maintaining Certification as a Hospice Nurse
To maintain certification as a hospice nurse, one must complete a recognized certification program, such as the Certified Hospice and Palliative Registered Nurse (CHPRN) or the Advanced Certified Hospice and Palliative Registered Nurse (ACHPRN) certification. These programs typically cover topics such as pain management, symptom control, and end-of-life care, as well as the emotional and spiritual support needs of patients and families. The certification process usually involves passing a written examination and completing continuing education requirements to maintain certification.
Value of Attending Conferences and Workshops
Attending conferences and workshops is an essential part of staying current in palliative care. These events provide a platform for hospice nurses to network with colleagues, learn from national leaders, and gain insight into the latest research, guidelines, and best practices in the field. Conferences and workshops often cover a range of topics, including pain management, symptom control, and end-of-life care, as well as best practices for providing emotional and spiritual support to patients and families.
- Network with colleagues and national leaders in the field
- Gain insight into the latest research and guidelines
- Learn from expert speakers and panelists
- Participate in hands-on training and simulations
Summary
As we conclude our exploration of hospice nurse jobs near me, it’s clear that these compassionate professionals play a vital role in providing end-of-life care. From the bedside to the office, hospice nurses work tirelessly to alleviate suffering and support patients and their loved ones during a difficult time. It’s essential to recognize the significance of these caregivers and the importance of their role in the healthcare system.
FAQ
What is the primary goal of hospice nursing?
The primary goal of hospice nursing is to provide comfort and alleviate suffering for patients with life-limiting illnesses.
What kind of education and training is required to become a hospice nurse?
Hospice nurses typically require an associate’s or bachelor’s degree in nursing, training in a hospice care program, and certification as a hospice and palliative care nurse.
What skills are essential for a hospice nurse to possess?
Empathy, effective communication, and emotional stability are crucial skills for hospice nurses to possess.
Can hospice nurses work from anywhere?
Hospice nurses often work in hospice care facilities or in the homes of patients, depending on their individual circumstances.