Interventional radiologists near me are specialized doctors that use minimally invasive procedures guided by imaging modalities to diagnose and treat a wide range of medical conditions.
They play a vital role in the healthcare system by providing alternative solutions to surgery, reducing morbidity and mortality rates, and improving patient outcomes. With advanced imaging technologies and techniques, interventional radiologists near me can perform a variety of procedures, from angioplasty and stenting to tumor ablation and biopsies.
The Process of Finding the Right Interventional Radiologist Near You
When it comes to finding the right interventional radiologist near you, there are several key factors to consider. This is crucial as it can impact the quality of care you receive and the success of your treatment plan. With so many options available, it’s essential to take the time to research and choose a qualified professional who meets your needs.
Credentials and Qualifications
Looking for a qualified interventional radiologist starts with checking their credentials. This includes verifying their medical licensing and board certification. In the United States, interventional radiologists must be certified by the American Board of Radiology (ABR) or the American Osteopathic Board of Radiology (AOBR). You can verify their credentials on the American Board of Medical Specialties (ABMS) or the American Osteopathic Association (AOA) websites.
Insurance Options and Affiliations
Another critical factor to consider is insurance coverage and hospital affiliations. Make sure the interventional radiologist is affiliated with a hospital that accepts your insurance plan. Additionally, confirm that the hospital is accredited by the Accreditation Council for Graduate Medical Education (ACGME) or the Joint Commission. This ensures that the hospital follows established standards for patient care and safety.
Patient Reviews and Ratings
Patient reviews and ratings can provide valuable insights into a physician’s skills and bedside manner. Look for online reviews on platforms like Healthgrades, RateMDs, or Vitals. However, keep in mind that online reviews can be biased and may not accurately reflect the physician’s quality of care. Consider reviews from multiple sources and look for a balanced perspective.
Referrals and Recommendations
Ask your primary care physician or a trusted family member or friend for recommendations. They may have personal experience with an interventional radiologist or know someone who has. Referrals can be a great way to get insider information and find a qualified professional who has a good reputation in the medical community.
Communication and Bedside Manner
Effective communication is critical when working with a healthcare professional. Look for an interventional radiologist who takes the time to answer your questions and listens to your concerns. A positive bedside manner can make a significant difference in your overall experience and comfort level during treatment.
Advanced Training and Specialist Expertise
Consider an interventional radiologist who has completed specialized fellowship training in the specific area of medicine they will be treating you for. This advanced training can provide the most up-to-date knowledge and skills to ensure the best possible outcome.
Language Barriers and Accessibility, Interventional radiologists near me
If you have a language barrier or require specialized care due to a medical condition, consider an interventional radiologist who speaks your language or has experience working with individuals with similar needs.
- Verify their medical licensing and board certification
- Check their hospital affiliations and insurance coverage
- Research patient reviews and ratings
- Ask for referrals and recommendations
- Evaluate their communication and bedside manner
- Consider advanced training and specialist expertise
- Assess language barriers and accessibility
Specialized Procedures and Techniques in Interventional Radiology: Interventional Radiologists Near Me
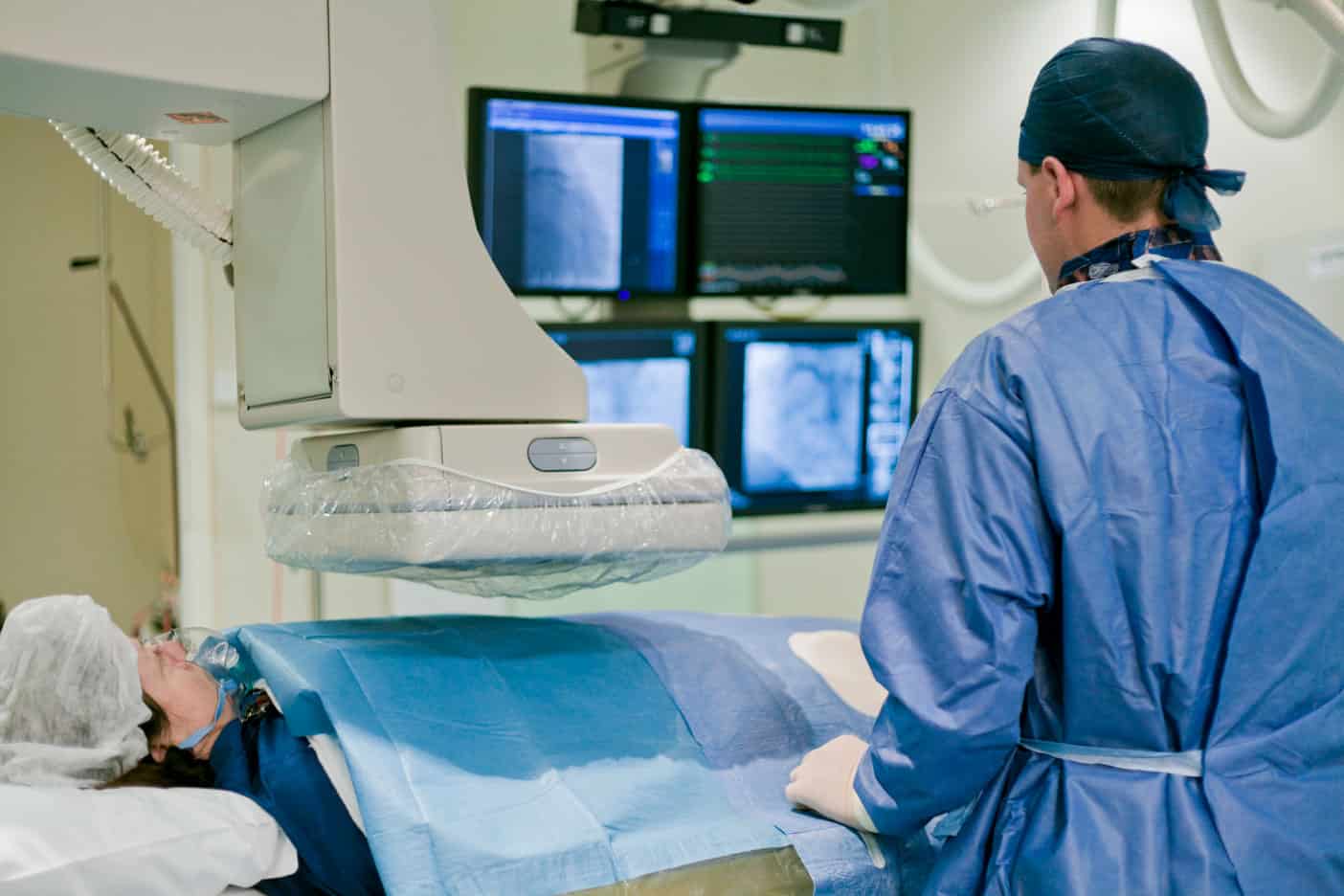
In the field of Interventional Radiology, various specialized procedures and techniques are employed to diagnose and treat a range of conditions. These procedures are typically minimally invasive, requiring only small incisions or no incisions at all, and offer a more precise and efficient alternative to traditional surgical methods. Among the most widely used techniques in Interventional Radiology are angioplasty and stenting for vascular interventions, tumor ablation using radiofrequency ablation, and microwave ablation.
Angioplasty and Stenting for Vascular Interventions
Angioplasty, also known as percutaneous transluminal angioplasty (PTA), is a procedure used to widen narrowed or blocked arteries using a balloon catheter. This is usually achieved by inflating a balloon at the end of the catheter, which pushes the blockage aside and helps restore blood flow. Stenting, on the other hand, involves placing a small metal mesh device, known as a stent, at the site of the blockage to keep it open and prevent re-narrowing.
In angioplasty, a catheter is inserted into the blocked artery through the femoral artery in the groin, and guided to the area of narrowing using fluoroscopy. A guidewire is then advanced through the catheter and across the blockage, with the balloon catheter following. The balloon is inflated to push the plaque and re-establish blood flow to the area. After the procedure, the balloon is deflated and removed, leaving the narrowed area widened.
A stent is typically left in place after angioplasty to keep the artery open and promote healing, while a stent can also be used in combination with angioplasty.
Tumor Ablation using Radiofrequency Ablation and Microwave Ablation
Tumor ablation is a technique used to destroy cancer cells by applying heat or cold temperatures to the targeted area. Two popular ablation methods are radiofrequency ablation (RFA) and microwave ablation (MWA). Both techniques involve the insertion of a thin needle into the tumor under imaging guidance, followed by the delivery of high-frequency electromagnetic energy to heat the surrounding tissue.
Radiofrequency Ablation (RFA)
RFA uses radiofrequency waves to heat cancer cells, causing them to die.
In RFA, a specialized electrode is inserted into the tumor and attached to a generator, which produces radiofrequency energy. The energy is then transferred to the tumor, causing the cells to heat up and die due to the denaturation of proteins. The extent of ablation can be monitored in real-time using imaging techniques such as ultrasound, CT scan, or MRI.
Microwave Ablation (MWA)
MWA uses microwave energy to heat cancer cells, causing them to die.
MWA involves the insertion of a microwave antenna into the tumor, which generates microwave energy. The microwave energy penetrates deep into the tumor, causing the cells to heat up and die due to the denaturation of proteins. MWA is particularly useful for treating larger tumors.
In RFA and MWA, the goal is to achieve complete ablation of the targeted tumor while minimizing damage to surrounding healthy tissue. These ablation techniques are often used in combination with other treatments, such as chemotherapy or surgery, to provide a more comprehensive approach to cancer treatment.
Advances in Imaging Technology for Improved Diagnostic Accuracy
Advances in imaging technology have significantly improved diagnostic accuracy in interventional radiology. The introduction of new imaging modalities such as contrast-enhanced ultrasound and MRI has enabled radiologists to obtain high-resolution images of internal structures, allowing for more accurate diagnoses and treatment plans.
One of the most significant advantages of contrast-enhanced ultrasound is its ability to provide real-time imaging of blood flow and tissue characteristics. This allows radiologists to monitor the effectiveness of treatments and make adjustments as needed. Additionally, contrast-enhanced ultrasound is less expensive and more widely available than other imaging modalities, making it an ideal choice for routine examinations.
Image-Guided Procedures
Image-guided procedures involve using imaging modalities to guide the placement of instruments or devices within the body. This technique has revolutionized the field of interventional radiology by allowing for minimally invasive procedures that reduce both risk and recovery time. Image-guided procedures are often used for biopsies, tumor ablations, and the delivery of chemotherapy directly to tumors.
Using image guidance during procedures minimizes the risk of complications and improves patient outcomes by allowing radiologists to:
- Obtain precise positioning of instruments and devices within the body
- Monitor the effectiveness of treatments in real-time
- Avoid damage to surrounding tissues and organs
This has significantly enhanced the accuracy and efficiency of interventional radiology procedures, making them a safer and more effective option for patients.
Advanced Imaging Modalities
In addition to contrast-enhanced ultrasound, advanced MRI technologies have also improved diagnostic accuracy in interventional radiology. These include:
- Functional MRI (fMRI): Measures blood flow and oxygenation to identify areas of the brain that are responsible for different functions
- Magnitude MRI: Provides high-resolution images of internal structures and detects subtle changes in tissue composition
These advanced imaging modalities have enabled radiologists to obtain detailed information about internal structures and diseases, allowing for more accurate diagnoses and treatment plans.
Ensuring Patient Safety in Interventional Radiology
Ensuring patient safety is of utmost importance in interventional radiology, where precise and delicate procedures are performed to diagnose and treat a variety of conditions. This specialized field requires a high level of expertise and precision, and interventional radiologists must adhere to strict protocols and guidelines to minimize the risk of complications and ensure the highest level of patient care.
To maintain patient safety, interventional radiologists employ various measures, including meticulous patient screening and selection, precise and accurate technique, and strict adherence to sterile technique and infection control protocols. Additionally, continuous education and training are vital to stay up-to-date with the latest techniques and technologies, allowing interventional radiologists to provide optimal care for their patients.
Proper Patient Positioning
Proper patient positioning is essential to ensure accurate and safe performance of interventional radiology procedures. This involves careful consideration of the patient’s positioning in relation to the anatomy involved, as well as consideration of factors such as access to the patient, equipment positioning, and monitoring.
- Patients are positioned in a comfortable and stable manner to minimize movement and discomfort during the procedure.
- The patient’s position is selected based on the specific anatomy involved, such as for vascular or liver procedures.
- Consideration is given to the positioning of equipment, such as fluoroscopy and radiation detectors.
Equipment Maintenance and Quality Control
The equipment used in interventional radiology procedures is critical to the success and safety of the procedure. Regular maintenance and quality control are essential to ensure that equipment is functioning properly and safely.
- Regular calibration and testing of equipment are performed to ensure accuracy and precision.
- Maintenance and repair of equipment are performed according to manufacturer’s instructions and guidelines.
- Quality control measures, such as image quality testing and radiation dose monitoring, are performed to ensure equipment is functioning safely and effectively.
Sterile Technique and Infection Control
Sterile technique and infection control are critical components of patient safety in interventional radiology. Interrnational radiologists must adhere to strict guidelines and protocols to minimize the risk of infection and ensure the highest level of patient care.
- Clean and sterile equipment is used throughout the procedure.
- Hands are washed and gloves are changed between patients to prevent cross-contamination.
- Patients receive antibiotics and other infection prevention measures as necessary.
Patient Monitoring and Support
Patient monitoring and support are vital components of patient safety in interventional radiology. Patients must be carefully monitored for signs of complications or adverse reactions during the procedure.
- Patients are continuously monitored for vital signs, such as heart rate, blood pressure, and oxygen saturation.
- Support teams, including nurses and anesthesiologists, are available to address any complications or concerns that arise during the procedure.
- Patients receive clear instructions and explanations throughout the procedure to minimize anxiety and ensure understanding.
Coordinated Care: Integrating Interventional Radiologists with Primary Care Physicians
Integrating interventional radiologists with primary care physicians is crucial for delivering high-quality patient care. By leveraging their expertise, patients receive comprehensive treatment that addresses the whole spectrum of their health needs. This collaborative approach ensures that interventional radiologists work in tandem with primary care physicians to create a seamless care continuum.
Communication and Coordination between Interventional Radiologists and Primary Care Physicians
Effective communication and coordination are the cornerstones of successful collaboration between interventional radiologists and primary care physicians. This involves clear and regular exchange of information, including:
- Diagnostic findings and test results
- Treatment plans and recommended interventions
- Post-procedure follow-up and monitoring
- Patient progress and any new developments
Regular communication enables primary care physicians to stay informed about patients’ treatment plans, reducing the likelihood of miscommunication or delays in care. Similarly, interventional radiologists benefit from primary care physicians’ expertise, particularly in evaluating and managing patients’ overall health.
Value of Multidisciplinary Care in Patient Management
Multidisciplinary care is essential in patient management, encompassing various healthcare professionals working together to deliver optimal outcomes. This collaborative approach extends beyond the confines of a single discipline, fostering a holistic understanding of patients’ needs. By integrating interventional radiologists with primary care physicians, patients receive:
- Comprehensive diagnostic evaluations
- Patient-centered treatment plans tailored to their unique needs
- Ongoing support and follow-up care
- Timely interventions and adjustments to treatment plans as needed
This approach recognizes that patient health is a complex, multifaceted issue that cannot be addressed by a single discipline or healthcare provider. Multidisciplinary care acknowledges the importance of collaboration and coordination in delivering high-quality patient care.
Collaborative Patient Management from Initial Diagnosis to Post-Procedure Follow-Up
Collaborative patient management involves primary care physicians, interventional radiologists, and other healthcare professionals working together to deliver comprehensive care. This continuum extends from initial diagnosis through treatment and post-procedure follow-up, with each stage requiring careful coordination and communication:
- Initial diagnosis and treatment planning: Primary care physicians consult with interventional radiologists to develop a comprehensive treatment plan.
- Procedural care: Interventional radiologists perform the procedure, while primary care physicians provide ongoing support and monitoring.
- Post-procedure follow-up: Primary care physicians work with interventional radiologists to monitor patient progress, address any complications, and adjust treatment plans as needed.
By maintaining a seamless line of communication and coordination throughout the care continuum, patients receive the highest level of care that addresses their unique needs and concerns.
Effective collaboration between interventional radiologists and primary care physicians can lead to improved patient outcomes, enhanced patient satisfaction, and reduced healthcare costs.
Expanding Access to Care
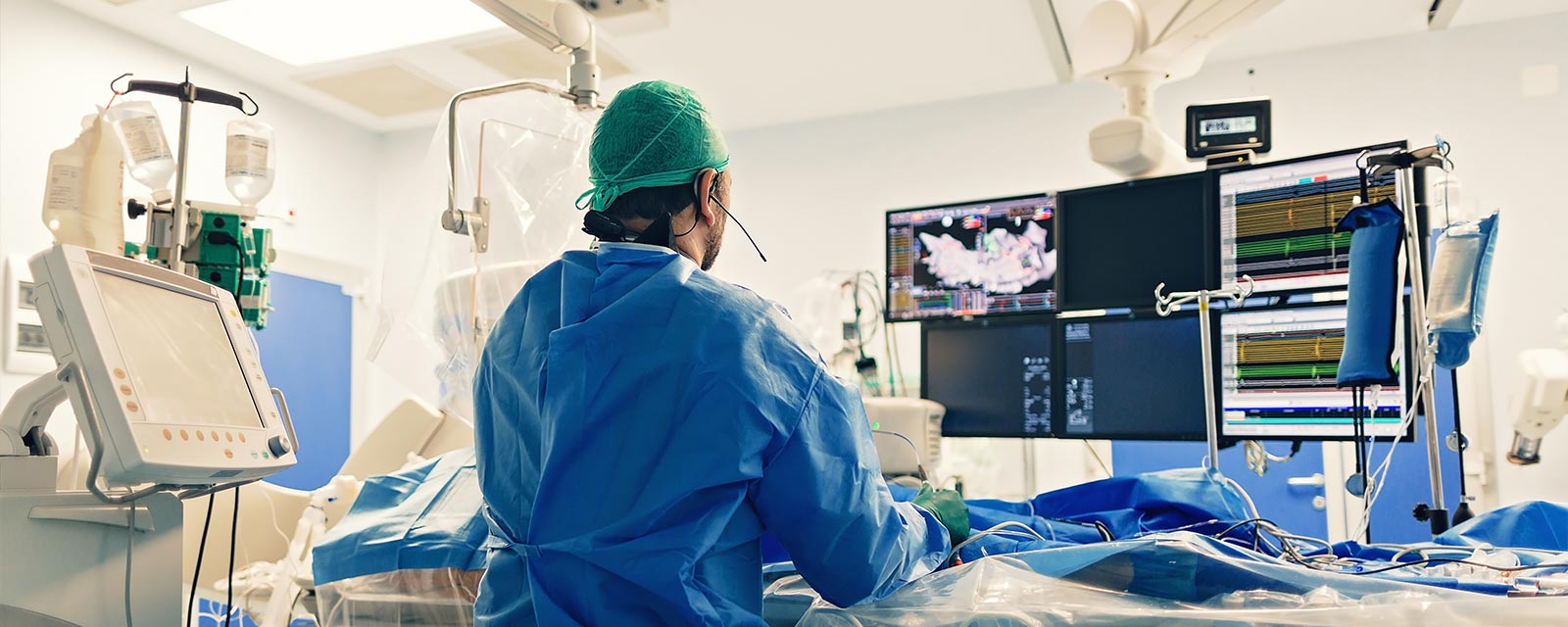
As the medical field continues to evolve, there’s been a growing trend of mobile radiology units and outreach services. This move towards accessible healthcare aims to bridge the gaps in healthcare services, particularly in rural or underserved areas where traditional medical facilities might be limited.
The Rise of Mobile Radiology Units
Mobile radiology units are custom-built vans or trucks equipped with imaging technology, such as X-ray, ultrasound, or CT scanners. These units enable medical professionals to travel to remote areas, conducting diagnostic imaging procedures in the field. By doing so, they provide timely access to medical care for patients who might otherwise face long wait times or travel to distant facilities.
Mobile radiology units offer several benefits:
- Improved diagnostic efficiency: By bringing imaging technology directly to patients, medical professionals can diagnose conditions more quickly, reducing the time patients spend in the hospital or on outpatient waitlists.
- Reduced emergency department utilization: Mobile radiology units can conduct urgent imaging procedures outside of emergency departments, freeing up hospital resources for more critical cases.
- Increased patient comfort: Mobile units can provide a more comfortable and familiar environment for patients, especially those with anxiety or phobias about medical imaging.
Mobile radiology units not only expand access to care but also help streamline healthcare resources. By providing timely diagnostic services, these units help prevent unnecessary hospital admissions, reducing healthcare costs and improving patient outcomes.
According to a study published in the Journal of the American College of Radiology, mobile radiology units have been shown to significantly reduce patient waiting times and emergency department utilization.
By investing in mobile radiology units and outreach services, healthcare systems can better serve their communities, providing timely access to medical care and improving overall health outcomes.
Building Strong Relationships with Patients

Effective communication and education are the foundation of strong relationships between interventional radiologists and their patients. By establishing trust and understanding, patients are more likely to adhere to treatment plans, manage their conditions, and achieve optimal outcomes. In this section, we will explore strategies for interventional radiologists to communicate treatment options and procedural risks to patients, as well as best practices for educating patients on post-procedure care and recovery.
Communicating Treatment Options and Procedural Risks
When presenting treatment options to patients, interventional radiologists must clearly and concisely explain the benefits, risks, and potential complications of each choice. This involves actively listening to patients’ concerns, values, and preferences, and tailoring communication to meet their individual needs. For instance, patients may feel more comfortable with certain procedures over others due to personal or cultural factors. By considering these factors, interventional radiologists can help patients make informed decisions about their care.
- Use simple, clear language to explain complex medical concepts: Avoid using technical jargon or medical jargon that patients may not understand. Instead, use plain language to explain procedures, risks, and benefits.
- Provide written information: Offer patients written information about their procedure, including risks, benefits, and post-procedure care. This helps them review information at their own pace and refer back to it as needed.
- Answer questions and address concerns: Create a safe and supportive environment where patients feel comfortable asking questions and expressing concerns.
- Use visual aids: Consider using visual aids, such as diagrams or images, to help patients understand complex medical concepts and procedures.
Educating Patients on Post-Procedure Care and Recovery
Patients must understand post-procedure care and recovery protocols to ensure a smooth and successful transition back to their daily lives. This includes managing symptoms, adhering to medication regimens, and participating in follow-up care. Interventions from interventional radiologists can help patients prepare for these next steps, reducing anxiety and stress associated with recovery.
- Provide personalized instructions: Offer patients tailored instructions on post-procedure care, including medication management, wound care, and activity limitations.
- Discuss signs of complications: Educate patients on potential signs of complications, such as excessive bleeding or infection, and emphasize the importance of seeking medical attention if they occur.
- Encourage follow-up care: Stress the importance of follow-up visits with primary care physicians or other specialists to monitor progress and address any concerns.
Clear communication and education are key to empowering patients and improving health outcomes. By working together, patients and interventional radiologists can build strong, trusting relationships that promote optimal care.
Conclusion
In conclusion, interventional radiologists near me offer a range of benefits, from reduced recovery times to improved diagnostic accuracy. By choosing the right interventional radiologist near you and understanding their specialized procedures and techniques, you can take control of your healthcare and make informed decisions about your treatment options.
FAQ Compilation
Q: What is the difference between an interventional radiologist and a conventional radiologist?
A: An interventional radiologist specializes in performing minimally invasive procedures guided by imaging modalities, whereas a conventional radiologist focuses on interpreting imaging studies and diagnosing conditions.
Q: How do I find the right interventional radiologist near me?
A: You can search online for interventional radiologists in your area, check their credentials and insurance options, and read patient reviews and ratings to make an informed decision.
Q: What are some common procedures performed by interventional radiologists near me?
A: Common procedures include angioplasty and stenting for vascular interventions, tumor ablation using radiofrequency ablation and microwave ablation, and biopsies to diagnose conditions.
Q: How do I prepare for a procedure with an interventional radiologist near me?
A: You should discuss your medical history, medications, and any concerns with your healthcare provider, follow pre-procedure instructions, and ask questions about the procedure and recovery process.