Neuro-ophthalmologists near me – Neuro-ophthalmologists undergo extensive training in both ophthalmology and neurology, allowing them to work effectively alongside neurosurgeons, neurologists, and other healthcare specialists to provide comprehensive care.
Neuro-ophthalmologists’ Unique Qualifications and Expertise in Eye Diseases
In the realm of ophthalmology, neuro-ophthalmologists stand at the forefront, bridging the intricate dance between the eye and the central nervous system. These highly specialized professionals undergo rigorous training to diagnose and treat a wide range of complex conditions, often serving as critical liaisons between ophthalmology and neurology departments.
Their expertise is forged through a unique blend of ophthalmic and neurological knowledge, allowing them to decipher the intricacies of eye diseases and their correlations with the brain, nervous system, and other bodily systems.
Advanced Training and Certifications
Neuro-ophthalmologists undergo extensive training, often spanning four to five years beyond medical school. They complete an ophthalmology residency program, followed by a fellowship in neuro-ophthalmology, which may last one to two years. This specialized training equips them with the skills to:
-
Diagnostic Techniques Specialized Skills Comprehensive eye exams, OCT scans, and visual field tests to assess vision and detect abnormalities. Interpretation of neuroimaging studies, such as MRIs and CT scans, to diagnose and monitor neurological and eye conditions. Advanced imaging techniques, like angiography and fluoroscopy, to visualize and diagnose blood vessel and eye conditions. Electrodiagnostic testing, including EMGs and VEPs, to evaluate nerve function and diagnose neuro-ophthalmic conditions. -
“Neuro-ophthalmologists must possess a deep understanding of both ophthalmic and neurological anatomy, physiology, and pathophysiology to accurately diagnose and treat complex conditions.” — American Academy of Ophthalmology (AAO)
-
Certifications Relevance American Board of Ophthalmology (ABO) certification in ophthalmology. Demonstrates expertise in comprehensive eye care, including diagnosis, treatment, and surgery. American Board of Ophthalmology (ABO) certification in neuro-ophthalmology. Highlights specialization in neuro-ophthalmic diagnosis, treatment, and management of conditions affecting the eye and central nervous system.
Collaboration with Healthcare Specialists
Neuro-ophthalmologists work closely with a multidisciplinary team of healthcare professionals, including neurosurgeons, neurologists, primary care physicians, and other specialists. Their unique expertise enables them to:
-
Provide precise diagnoses, taking into account the intricate relationships between the eye and central nervous system.
-
Develop and implement comprehensive treatment plans, integrating the latest research and evidence-based medicine.
-
Offer expert consultation and advice to colleagues, ensuring seamless coordination of care for patients with complex conditions.
Identifying and Treating Eye Symptoms in Neurological Disorders

In the realm of neuro-ophthalmology, a delicate dance between the eyes and the brain unfolds. Neuro-ophthalmologists, with their unique expertise, navigate this intricate landscape to identify and treat eye symptoms that betray the presence of neurological disorders. The consequences of misdiagnosis or delayed treatment can be dire, yet a neuro-ophthalmologist’s specialized knowledge empowers them to provide compassionate care.
Eye Symptoms Associated with Multiple Sclerosis
Multiple sclerosis, a chronic autoimmune disease, often manifests with ocular symptoms that signal the involvement of the central nervous system. Neuro-ophthalmologists recognize the importance of promptly identifying these symptoms, which may include:
- Optic neuritis, an inflammation of the optic nerve that can cause vision loss, pain, and sensitivity to light.
- Double vision, resulting from damage to the nerves that control eye movement.
- Blurred vision, a symptom that can arise from inflammation or damage to the optic nerve or surrounding tissues.
- Nystagmus, an involuntary movement of the eyes that can indicate cerebellar dysfunction.
In multiple sclerosis, these ocular symptoms can be harbingers of neurological involvement, underscoring the importance of meticulous examination and diagnosis. Neuro-ophthalmologists play a vital role in diagnosing and managing these symptoms, ensuring that patients receive timely and effective treatment.
Eye Symptoms Associated with Parkinson’s Disease
Parkinson’s disease, a neurodegenerative disorder, often presents with a range of ocular symptoms that reflect its impact on the brain and nervous system. Neuro-ophthalmologists are adept at recognizing these symptoms, which may include:
- Microphthalmos, a condition characterized by abnormally small eyes, which can be a manifestation of Parkinson’s disease.
- Lid retraction, a situation in which the eyelids are abnormally high due to increased sympathetic tone.
- Diplopia, a symptom of oculomotor nerve palsy, which can be a result of Parkinson’s disease.
- Dilated pupils, which can be a sign of autonomic dysfunction in Parkinson’s disease.
In Parkinson’s disease, these ocular symptoms can signal the progression of the disease and the need for closer monitoring and management. Neuro-ophthalmologists collaborate with neurologists to ensure a comprehensive approach to care, addressing both the ocular and neurological implications of the disease.
Eye Symptoms Associated with Stroke or Transient Ischemic Attack
Stroke and transient ischemic attack (TIA), conditions characterized by temporary or permanent interruption of blood flow to the brain, frequently manifest with ocular symptoms that signal their presence. Neuro-ophthalmologists are well-versed in recognizing these symptoms, which may include:
- Visual field loss, which can result from damage to the occipital lobe or optic tract.
- Homonymous hemianopia, a condition in which one half of the visual field is lost due to damage to the optic tract or occipital lobe.
- Monocular blindness, a symptom that can arise from central retinal artery occlusion or other vascular events.
- Posterior communicating artery syndrome, a condition characterized by visual disturbances and extraocular muscle paralysis.
In stroke or TIA, these ocular symptoms can herald the importance of prompt evaluation and treatment. Neuro-ophthalmologists contribute to the diagnostic process, providing critical information that aids in the timely identification and management of these conditions.
Recent Advances in Neuro-ophthalmology for Conditions Like Glaucoma and Macular Degeneration
In a field where every passing minute matters, recent advances in neuro-ophthalmology have brought hope to those struggling with glaucoma and macular degeneration. Innovative treatments and technologies, once considered science fiction, are now becoming a reality.
Surgical Procedures for Glaucoma
Surgical procedures have come a long way in treating glaucoma, a condition where increased eye pressure damages the optic nerve. Minimally invasive glaucoma surgery (MIGS) has reduced the trauma to the eye, allowing for quicker recovery times and less risk of complications.
MIGS includes procedures like trabecular micro-bypass, ab-interno circumferential trabeculotomy, and suprachoroidal stent implantation.
- Trabecular Micro-Bypass: This procedure involves implanting a small device in the trabecular meshwork, allowing fluid to drain from the eye more efficiently. By reducing eye pressure, it slows the progression of glaucoma.
- Ab-Interno Circumferential Trabeculotomy: This minimally invasive procedure involves making a small incision in the eye and then inserting a specialized instrument to create a new drainage pathway in the trabecular meshwork.
- Suprachoroidal Stent Implantation: This procedure involves placing a small stent between the sclera and the choroid, allowing for faster drainage of fluid from the eye.
Emerging Technologies for Macular Degeneration
Macular degeneration, a leading cause of vision loss in the elderly, has seen significant advancements in recent years. Emerging technologies like optogenetics, gene therapy, and nanotechnology hold promise for treating this debilitating condition.
Optogenetics involves using light to control gene expression in specific cells, allowing for targeted treatment of macular degeneration. Gene therapy introduces healthy copies of a gene to replace faulty ones, reducing the risk of vision loss. Nanotechnology has led to the development of targeted delivery systems for treatments, reducing side effects and increasing efficacy.
- Optogenetics: This innovative approach involves implanting a device that uses light to stimulate cells in the retina, bypassing damaged photoreceptors and restoring vision.
- Gene Therapy: This treatment introduces healthy copies of the RPE65 gene to replace faulty ones, reducing the risk of vision loss in those suffering from Leber congenital amaurosis.
- Nanotechnology: This technology has led to the development of targeted delivery systems for treatments, such as nanoparticles and micelles, which can selectively target damaged areas of the retina, reducing side effects and increasing efficacy.
Predictions for Future Breakthroughs
While advancements in neuro-ophthalmology have been significant, we can expect even more cutting-edge treatments and technologies in the near future. Predictions include the use of artificial intelligence, robotics, and personalized medicine to better diagnose and treat glaucoma and macular degeneration.
The Role of Neuro-ophthalmologists in Conducting Neuroimaging Studies: Neuro-ophthalmologists Near Me
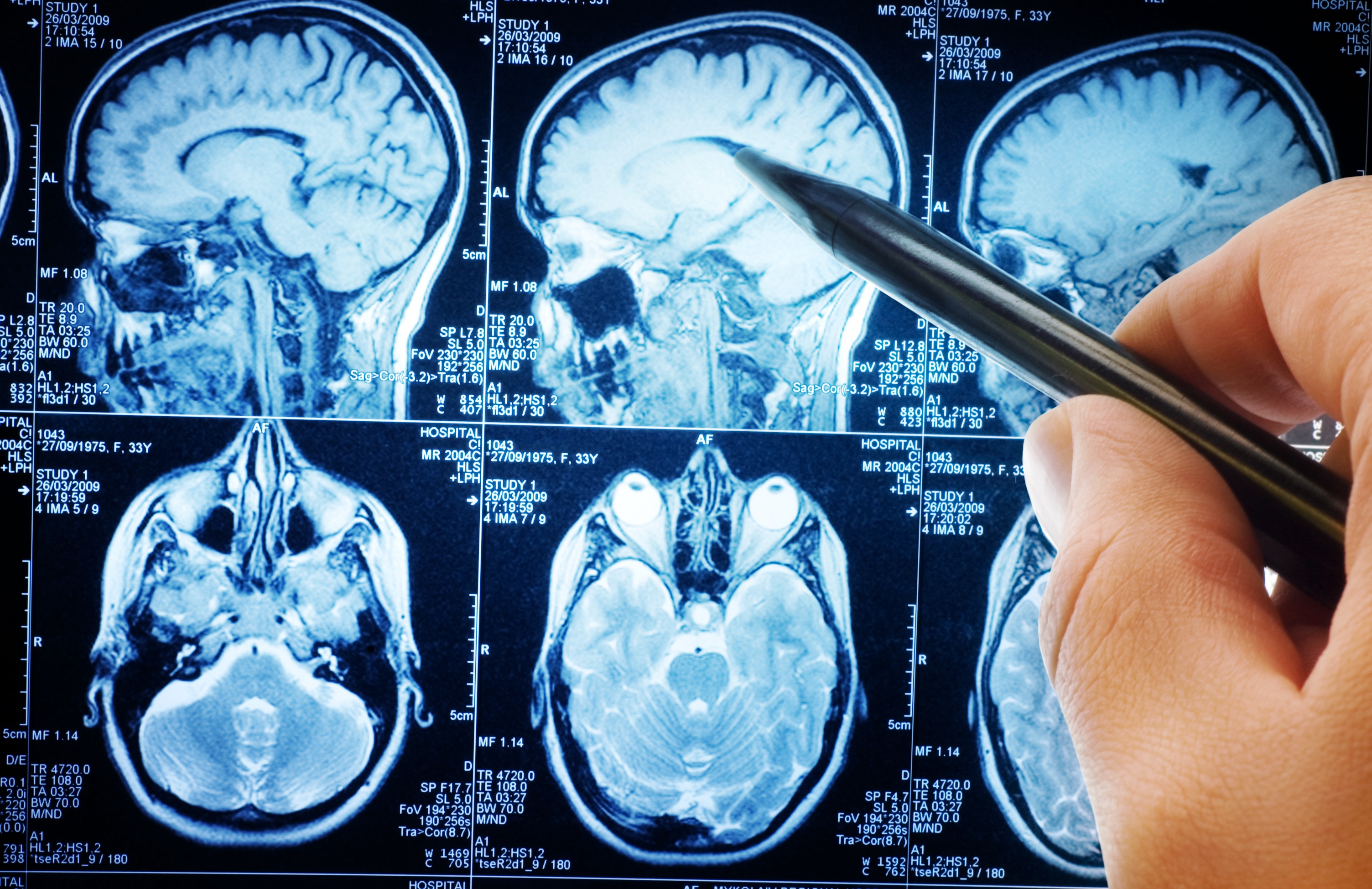
In the realm of neuro-ophthalmology, the intersection of eye diseases and neurological disorders demands a unique combination of expertise. Neuro-ophthalmologists bridge this gap by employing neuroimaging studies to unravel the complexities of their patients’ conditions. At the heart of this endeavor lies the skillful interpretation and analysis of images from advanced imaging modalities such as MRI and CT scans.
Within the realm of image interpretation, neuro-ophthalmologists must grapple with the intricacies of neural and ocular anatomy. Each scan offers a glimpse into the hidden structures that govern our visual and cognitive abilities, providing a window onto potential maladies. This delicate task necessitates a profound understanding of the neuro-ophthalmic connection, a symbiosis that only experienced practitioners can decipher.
Interpreting MRI and CT Scans
In the world of neuroimaging, MRI and CT scans stand as sentinel markers for disease diagnosis. By combining these modalities, neuro-ophthalmologists acquire a multifaceted view of their patients’ conditions, a mosaic of symptoms that only careful interpretation can unravel. The nuances of each scan – from the fluid dynamics of the cerebrospinal fluid to the retinal detachment’s subtle topography – serve as a testament to the intricate relationships between the brain, eyes, and nervous system.
The art of image interpretation demands more than technical proficiency; it necessitates compassion, patience, and an empathetic touch. Neuro-ophthalmologists must translate the silent whispers of the scan into a clear and actionable diagnosis, a verdict that guides treatment and sets a patient’s path towards healing.
Key Characteristics of the Best Neuro-ophthalmology Clinics and Specialists

In the realm of eye and brain conditions, a delicate balance between art and science is required. A neuro-ophthalmologist’s keen mind and skilled hands navigate the intricate dance between vision and neurology, making their expertise a treasure trove for those seeking relief from these complex ailments.
When seeking out the best neuro-ophthalmology clinics and specialists, one must look for those who embody a unique blend of skills and qualities. It is the combination of a deep understanding of both eye and brain conditions, alongside a passion for delivering cutting-edge care, that sets apart the exceptional from the merely good.
Essential Qualities of an Effective Neuro-ophthalmologist
A truly exceptional neuro-ophthalmologist is one who is equally at home in both the eye and brain worlds. Their expertise should be reflected in their ability to seamlessly transition between the two, leveraging a deep understanding of both to deliver the most effective care possible. This requires not only a broad knowledge base but also a keen eye for the subtle nuances that can make all the difference in diagnosis and treatment.
Key components of a reputable neuro-ophthalmology clinic include:
- Comprehensive Diagnosis and Treatment Options: A good neuro-ophthalmologist should be equipped to diagnose and treat a wide range of conditions affecting the eyes and brain, from common problems like glaucoma to more complex conditions requiring interdisciplinary care.
- Collaborative Care Team: For optimal patient outcomes, a neuro-ophthalmologist often works closely with other specialists, including neurologists, ophthalmologists, and other medical professionals. Look for clinics where this collaborative approach is a cornerstone of their care model.
- State-of-the-Art Diagnostic Equipment: To accurately diagnose and treat complex conditions, the latest diagnostic technologies are essential. Ensure the clinic has access to cutting-edge equipment, such as advanced imaging and diagnostic tools.
- Personalized Care and Treatment Planning: A leading neuro-ophthalmologist will take the time to understand each patient’s unique needs and develop a treatment plan tailored to their specific health status and goals. This requires excellent patient communication and a willingness to adapt to changing circumstances.
- Continuing Education and Professional Development: The medical field is constantly evolving, and the best neuro-ophthalmologists stay up-to-date with the latest research, treatments, and technologies through ongoing education and training.
In the realm of neuro-ophthalmology, seeking out clinics and specialists who embody these qualities is a vital step in ensuring access to the highest level of care.
It is the convergence of expertise, collaboration, cutting-edge technology, patient-centered care, and ongoing education that defines the best neuro-ophthalmology clinics and specialists. When choosing where to seek care, it is critical to look for these distinguishing characteristics, as they are the hallmark of excellence in this complex and rapidly evolving field.
Managing Eye Health during Rehabilitation from Neurological Injuries or Illnesses
As the road to recovery unfolds, patients with neurological injuries or illnesses face an array of challenges that span far beyond their physical rehabilitation. Eye health, an often-overlooked aspect of overall well-being, plays a vital role in their progress and success. Neuro-ophthalmologists, experts in the unique intersection of neurology and ophthalmology, stand at the forefront of managing eye health during this critical period.
The Critical Role of Neuro-ophthalmologists in Rehabilitation
Neuro-ophthalmologists are uniquely positioned to address the complex interplay between neurological and ophthalmological conditions. Their expertise enables them to identify and address vision-related issues that may be contributing to or compounding the patient’s recovery. By integrating their knowledge of neurological and ophthalmological principles, they can provide comprehensive care that addresses the multifaceted needs of patients undergoing rehabilitation.
Enhancing Vision and Preventing Secondary Complications, Neuro-ophthalmologists near me
To optimize the rehabilitation process, neuro-ophthalmologists employ a range of techniques that focus on enhancing vision and preventing secondary complications. These techniques may include:
Visual rehabilitation therapy, which aims to restore and adapt vision to compensate for neurological damage, has been shown to significantly improve visual function and quality of life in patients with stroke and traumatic brain injury.
- Low vision rehabilitation, which involves the use of specialized devices and strategies to help patients adapt to vision loss and optimize their remaining vision.
- Cognitive training, which targets attention, memory, and executive function to enhance visual perception and improve overall cognitive function.
- Eye movement training, which helps patients regain control over their eye movements and improve their ability to track and follow objects.
- Pain management and rehabilitation, which focuses on reducing pain and discomfort associated with eye movements and visual function.
Collaboration and Coordinated Care
Effective management of eye health during rehabilitation depends on close collaboration among neuro-ophthalmologists, rehabilitation therapists, and other healthcare professionals. By working together, they can provide comprehensive care that addresses the complex needs of patients and facilitates their recovery.
A well-coordinated approach may involve:
- Therapeutic interventions, such as vision therapy and cognitive training, which are tailored to the individual’s specific needs and goals.
- Collaborative assessment and monitoring of visual function and any related complications.
- Regular communication and updates among healthcare providers to ensure seamless integration of care.
- Patient education and support to empower individuals to take an active role in their recovery.
Final Wrap-Up
In conclusion, finding a neuro-ophthalmologist near you can make a significant difference in your healthcare journey. With their specialized expertise and advanced training, you can trust that your eye and brain conditions will receive the best possible care.
Key Questions Answered
What qualifications do neuro-ophthalmologists have?
Neuro-ophthalmologists undergo specialized training in both ophthalmology and neurology, including residency programs and fellowship training. They also have certifications from professional organizations such as the American Academy of Neurology.
How do neuro-ophthalmologists diagnose eye symptoms related to neurological disorders?
Neuro-ophthalmologists use a combination of clinical evaluation, imaging studies (such as MRI and CT scans), and laboratory tests to diagnose eye symptoms related to neurological disorders. They also work closely with other healthcare specialists to provide a comprehensive diagnosis and treatment plan.
What are some recent advances in neuro-ophthalmology for conditions like glaucoma and macular degeneration?
Recent advances in neuro-ophthalmology include the development of new surgical procedures, medical devices, and imaging technologies to diagnose and treat glaucoma and macular degeneration.
How do neuro-ophthalmologists contribute to the diagnosis and management of neurological disorders?
Neuro-ophthalmologists play a critical role in the diagnosis and management of neurological disorders, including multiple sclerosis, Parkinson’s disease, and stroke. They work closely with other healthcare specialists to provide a comprehensive treatment plan and follow-up care.